Oral Herpes (Cold Sores, Fever Blisters) Treatment and Prevention
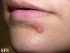
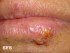
Oral herpes or mouth herpes is caused by the Herpes simplex type 1 virus (HSV-1). Also known as cold sores or fever blisters, this infection has a tendency to recur several times in life and the infection remains latent and therefore asymptomatic in between. A recurrence is referred to as a reactivation while the first time a person is infected is known as the primary infection.
Despite the most aggressive treatment during the primary infection, reactivation and a recurrence of the symptoms is unavoidable. However, the symptoms are usually much milder in a recurrence than it is with the primary infection. Many of the symptoms like a fever, shallow ulcers, headache and lymphadenopathy (swollen lymph nodes) seen along with the fluid-filled blisters (vesicles) in the primary infection is absent – patients may only report the solitary vesicle or a small group vesicles in a recurrence.
Diagnosis of Oral Herpes
It is important to first be diagnosed with oral herpes which is known as acute herpetic gingivostomatitis or recurrent herpetic stomatitis. Other viral infections of the oral cavity and around the mouth may include cytomegolovirus (CMV), Epstein-Barr (EBV), herpes zoster and measles.
The clinical history with a consideration of the signs, symptoms and duration is often used for differential diagnosis prior to laboratory testing. Apart from taking tissue samples and fluid from the vesicles for testing, a viral culture analysis can be done and there are blood tests (antigen-antibody) to identify whether the infection is caused by HSV-1 or HSV-2.
Treatment of Oral Herpes
It is important to note that treatment should be started as early as possible even before the appearance of visible lesions on the skin, lips or in the oral cavity. Despite treatment, a recurrence cannot be avoided altogether.
Topical
A topical antiviral cream, ointment, solution or gel containing penciclovir or docosanol may be used as early as possible to limit the discomfort and duration of the disease. It can be started before the typical cold sore/fever blister is visible as the lesion itself is preceded by a period of tingling, itching or burning pain at the site.
A topical anesthetic containing benzocaine or a mouthwash with lidocaine may be considered for pain relief in the event of severely painful blisters. However, this should be prescribed by a doctor and may not be advisable in the event of deep ulcers.
Medication
Oral antiviral agents are usually not necessary and only prescribed in severe cases. It is typically not used for mouth herpes despite being a fairly effective treatment. These drugs contain acyclovir, valacyclovir or famciclovir. Acyclovir is widely used both for primary infection and a recurrence. A virus may become resistant to acyclovir and other antiviral agents like foscamet may then be used. However this is not usually necessary for oral herpes.
Pain relieving medication may be used for painful cold sores. However this is often not necessary and should be used minimally.
Prevention for Oral Herpes
Primary infection is often difficult to avoid as vesicles in the mouth may not be visible. A recurrence can be prevented to some extent or at least limited. The preventative measures revolve around avoiding trigger factors and practicing good personal hygiene.
- Avoid kissing or sharing kitchen utensils with a person who has visible cold sores/fever blisters. Even in the early phase where no skin lesion is visible but there is tingling or itching can be a contagious stage.
- Wash hands frequently when making contact with a person who has cold sores. Avoid sharing towels and personal items.
- Avoid touching certain areas particularly the eyes, mouth and genitals of an infected person. The involvement of HSV-2 in oral herpes has raised the concern about sexual transmission although HSV-1 is rarely associated with sexual contact.
- Recurrence may be limited by avoiding trigger factors. Although the process behind this reactivation is poorly understood and recurrence is usually mild, there are several trigger factors that have been identified including trauma, allergies, certain foods and ultraviolet light exposure. Pregnancy and menstruation which are known trigger factors are unavoidable.
- A weak immune system is also a factor to consider in a recurrence and this is under a person’s control to a certain extent – eat a healthy diet, exercise, minimize stress and ensure that chronic conditions like diabetes mellitus is properly treated and appropriately managed. Patients with immunodeficiency like HIV-positive and AIDS patients should be more attentive to personal hygiene and contact with others.
- Sunlight has come to the forefront of triggering a recurrence on the lips and around the mouth. The effect of sunlight exposure can be minimized with the use of sunblock on the skin and lip balms containing UV protection.
- Keep the area clean. A secondary bacterial infection can arise especially when the cold sore / fever blister ruptures and leads to an ulcer.