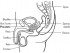
Prostatitis (Prostate Gland Infection)
What is prostatitis?
Inflammation of the prostate gland is known as prostatitis. It may be caused by an infection but there are other non-infectious causes that may also be responsible. Infectious causes of prostatitis are less frequently seen. The non-infectious causes of prostatitis are often chronic and more complex than infectious prostatitis.
Types of Prostatitis
Prostatitis can be categorized as acute or chronic bacterial prostatitis (infectious) or chronic abacterial prostatitis and granulomatous prostatitis. The more widely used classification for prostatitis these days is as follows :
- Acute bacterial prostatitis
- Chronic bacterial prostatitis
- Chronic prostatitis and chronic pelvic pain syndrome (CPPS), which may be inflammatory or non-inflammatory
- Asymptomatic inflammatory prostatitis
Simply, prostatitis can be divided into infectious and non-infectious.
Acute and Chronic Bacterial Prostatitis
Most prostate gland infections are due to bacteria, although viral prostatitis which is rare may be seen in immunocompromised patients like those with HIV infection. Bacterial prostatitis is usually seen when other prostate disorders, like benign prostatic hyperplasia, are present. The infection may be acute or chronic and is usually superimposed over the existing prostate problem.
Bacteria may travel up the urethra to reach the prostate gland or travel in the urine and pass through the prostatitic ducts to infect the prostate tissue. In other cases the bacteria may reach the prostate gland from surrounding tissues like direct infiltration from the neighboring rectum. Alternatively the bacteria may reach the prostatic tissue through the blood stream (hematogenous spread) or lymphatic system. Read more on prostate gland infection.
Chronic Prostatitis (Chronic Pelvic Pain Syndrome) and Asymptomatic Inflammatory Prostatitis
Non-infectious prostatitis may be inflammatory or non-inflammatory. Despite the fact that prostatitis means prostate inflammation, the non-inflammatory cases are termed as such due to the absence of inflammatory cells in the urine or semen.
Non-infectious prostatitis is often chronic and may appear repeatedly and resolve, often without treatment. Infections of the prostate gland frequently arise in these cases. Non-inefctious prostatitis is often associated with pain and even in instances where the prostate gland is not inflamed, pain may still be present possibly as a result of nerve injury (chronic pelvis pain syndrome). Some cases of non-infectious prostatitis may be silent (asymptomatic) despite the presence of inflammatory cells in the urine and semen.
Causes of Prostate Gland Infection
Most prostate gland infections are due to bacteria. Rarely, viral and fungal prostatitis may occur although it is more often associated with immunocompromised states. Bacterial prostatitis is less common than other non-infectious causes. In acute prostatitis, usually the same bacteria that are involved in urinary tract infections may also infect the prostate. This includes E.coli, enterococci and staphylococci. With chronic prostatitis, however, the are a host of microorganisms that may also play a role in infection, including Klebsiella spp, Enterobacter spp, staphylococci, Pseudomonas spp and enterococci.
The microorganisms gain entry into the prostatic tissue through multiple routes. The most common is when microorganisms enter through the penile urethra and spread up the urinary tract. This is known as an ascending urethral infection. Microorganisms in the urine may also enter the prostatitic ducts, against the regular flow of urine. This is known as reflux of infected urine. In acute prostatitis, these routes of transmission are usually responsible.
Bacterial prostatitis may also arise through direct infiltration of the rectal bacteria. Lymphatic spread of the rectal bacteria and hematogenous spread of bacteria through the blood stream from distant sites may also be responsible.
Signs and Symptoms of Prostate Gland Infection
The symptoms of acute bacterial prostatitis are usually intense while in chronic cases, the presentation may be mild or even asymptomatic.
- Frequent urination
- Painful urination (dysuria)
- Difficulty passing urine
- Perineal pain or groin pain – may also involve the penis and scrotum
- Low back ache
- Tenderness, warmth and swelling of the prostate gland may be more evident in acute bacterial prostatitis
- Fever and chills are more frequently seen in acute bacterial prostatitis
- Malaise, arthralgia (joint pain) and myalgia (muscle pain) are usually indicate of an acute infection
- Sexual dysfunction is more likely to arise with chronic bacterial prostatitis and patients may also report pain during ejaculation.
The risk of developing a prostatitic abscess exists especially with acute bacterial prostatitis and may require drainage.
Diagnosing Bacterial Prostatitis
Laboratory tests are useful for conclusively diagnosing bacterial prostatitis and identifying the causative microorganism. However it should be assessed in conjunction with findings upon conducting a physical examination. The presence of prostatitis symptoms need to be carefully recorded and considered along with a patient’s medical history. A rectal examination will reveal a swollen and firm prostate gland with the patient reporting tenderness.
Urine cytology and urine culture should be considered for acute bacterial prostatitis. The sample should reveal more than 10 white blood cells per high power field (WBCs/HPF) along with a positive bacterial culture. The presence of white blood cells on its own is indicative of inflammation but non-specific for infection.
Expressed prostatic secretions (EPS) should be submitted for cytology and culture in chronic bacterial prostatitis. A sample with more than 10 WBCs/HPF (leukocytosis) and a positive bacterial culture would be indicative of infectious prostatitis. A PSA level may be done at the outset and a follow up test repeated 6 to 8 weeks after starting treatment to ensure that levels are decreasing. It is not used as an diagnostic indicator for prostatitis specifically. Elevated PSA levels, despite resolution of prostatitis symptoms following treatment, will prompt further investigation to exclude prostate cancer. This may involve imaging studies and a prostate biopsy.
Treatment of Bacterial Prostatitis
Both acute and bacterial prostatitis are treated with antibiotics (oral) although more severe cases may require IV administration. Antibiotic use for bacterial prostatitis often spans a longer period of time and compliance is essential for resolution of the infection without complications.
The types of antibiotics used for bacterial prostatitis includes :
- Ciprofloxacin
- Ofloxacin
- Levofloxacin
- Trimethoprim-sulfamethoxazole
These antibiotics have better epithelial penetration and therefore using other antibiotics may not be as effective. Surgical drainage may be considered when complications like a prostate abscess arises but this is rare.