The Prostate Gland – Problems, Diseases, Tests
The prostate gland, which lies below the bladder and surrounds the urethra, is the male organ that produces semen. It is very common for the prostate gland to start enlarging after the age of 40, although it may not always produce symptoms. The first noticeable symptoms appear when the enlarged prostate gland presses upon the urethra, causing problems with urination. The most common problems encountered with the prostate are benign prostatic hyperplasia (BPH), prostate cancer and prostatitis.
Anatomy & Physiology of the Prostate Gland
The prostate gland is about the size of a pea at birth, growing slowly in childhood, but undergoes rapid development at puberty. It becomes the size of a walnut by the age of 25, when it is thought to be fully developed.
The prostate gland lies below the bladder, wrapped around the urethra (the tube that drains urine from the bladder), between the pubic bone and the rectum. It is slightly conical in shape, consisting of a base, an apex, an anterior (front), a posterior (rear), and two lateral (side) surfaces. It is partly muscular and partly glandular and is surrounded by a thick capsule.
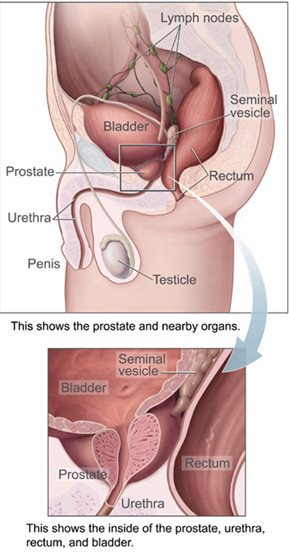
The prostate gland is divided into several lobes, namely :
- a median lobe or middle lobe
- two lateral lobes on either side
- an anterior lobe in the front
- a posterior lobe at the back
The prostate may also be divided into zones according to their function :
- central zone
- peripheral zone
- transitional zone
The prostatic ducts open into the prostatic part of the urethra (the part of the urethra lying within the prostate). The two ejaculatory ducts from the seminal vesicles enter the prostate at its upper border and the prostatic part of the urethra merges with them.
The male urethra conducts two functions :
- It allows passage of urine from the bladder during urination.
- It also carries semen during ejaculation.
The prostate gland produces components of semen which helps to nourish and transport sperm during ejaculation. This milky white fluid, slightly alkaline in composition, also helps to neutralize the acidic environment of the vaginal tract and thus helps in prolonging the life span of the sperm. The prostatic secretion consists of alkaline phosphatase, citric acid, prostate-specific antigen (PSA), and proteolytic enzymes. The male hormone, testosterone, is necessary for proper functioning of the prostate gland.
Enlargement or hyperplasia of the prostate occurs when cells in the central portion of the gland start multiplying, which may compress the urethra, causing difficulty in passing urine.
Prostate Diseases
The clinical problems associated with the prostate gland may be divided into two categories :
1. Benign or non-cancerous prostate problems
2. Prostate cancer
Benign or Non-Cancerous Prostate Problems
- Benign prostatic hyperplasia (BPH) or enlarged prostate is the most common non-cancerous prostate problem that is encountered.
- Prostatitis is the inflammation of the prostate gland, which may cause symptoms such as pain, discomfort, frequent urination, and fever. Prostatitis may be categorized into four types :
- Acute bacterial prostatitis
- Chronic bacterial prostatitis
- Chronic non-bacterial prostatitis / chronic pelvic pain
- Asymptomatic inflammatory prostatitis
- Prostatism includes any condition of the prostate which interferes with the passage of urine from the bladder.
- Prostalgia is pain in the prostate gland.
Prostate Cancer
Cancer of the prostate gland is one of the most common types of cancer in men and is more prevalent in the older age group. It most frequently remains symptomless in the initial stages, but there may be urinary symptoms similar to those of benign prostatic hyperplasia. Early detection and treatment gives better chance of survival.
Tests & Procedures to Assess Prostate Problems
- History and physical examination of the patient.
- Digital rectal examination is when a gloved, lubricated finger is inserted gently into the rectum. The doctor will be able to determine any enlargement of the prostate gland, as well as indicate any signs of prostate cancer.
- Urine test is conducted to rule out urine infection and other conditions that may cause symptoms similar to those seen in BPH, such as prostatitis, bladder infection or kidney disease.
- Prostate-specific antigen (PSA) blood test. PSA is produced in small amounts by the normal prostate gland, but a higher than normal value or an excessively high value of PSA in the blood should alert the physician to the possibility of BPH or prostate cancer.
- Transrectal ultrasound (TRUS) may be done to determine the size of the prostate gland and to rule out prostate cancer.
- Urodynamic pressure-flow studies may need to be done in patients with complicated urinary symptoms, to measure bladder pressure and function, as well as urinary flow.
- Cystoscopy may be done to visualize the inside of the bladder and urethra, to diagnose any compression of the urethra by an enlarged prostate. It can also help to determine if there is any blockage of the urethra or bladder neck, bladder stone or any anatomical abnormality.
- Intravenous pyelogram (IVP) or CT urogram is when an x-ray or CT scan is done after injecting a dye into a vein, to find any obstruction or abnormality in the urinary tract.
- Urinary flow test measures the strength and amount of urine flow and may indicate prostate or bladder problem.
- Postvoid residual volume test is done to determine whether complete emptying of the bladder is taking place and to measure the amount of urine left in the bladder after urination.
- Biopsy. A small tissue sample is removed for microscopic examination to detect or rule out prostate cancer. A large hollow needle may be used to remove a plug of tissue in traditional biopsy, or the tissue may be removed through fine needle aspiration.