Tinea Nigra (Black Fungus on Palm or Sole) Information and Pictures
What is tinea nigra?
Tinea nigra is a fungal infection that is mainly seen on the palms of the hands or soles of the feet causing a dark brown to black discoloration of the affected skin. The word tinea means a fungal infection and nigra means black. Tinea nigra is overall an uncommon fungal infection when compared to other tinea infections like tinea pedis (feet but usually not the soles), tinea cruris (groin), tinea capitis (scalp) and tinea corporis (body). Most of these other tinea infections are caused by similar species of skin fungi which are commonly found in the environment but tinea nigra is due to rather uncommon fungal species.
Tinea nigra is a superficial dermatomycosis meaning that the fungal infection of the skin is limited to the outermost layers. The fairly benign presentation with no itching or skin inflammation means that secondary bacterial infections and permanent scarring are rare. Tinea nigra is more commonly seen in children and is more likely in girls than boys. The conditions also tends to affect lighter skinned individuals than darker skinned people.
Tinea Nigra Causes
Tinea nigra is a superficial fungal infection caused by one of the following fungi :
- Phaeoannellomyces werneckii – more common causative agent of tinea nigra.
- Stenella araguata
- Cladophialophora saturnica
Phaeoannellomyces werneckii is also known by several other names including :
- Hortaea werneckii
- Exophiala werneckii
- Cladosporium werneckii
Phaeoannellomyces werneckii is a brown mold that is found in soil, compost and on wood (geophilic fingi). This species of fungi is generally found in humid tropical and sub-tropical regions particularly in South America, Africa, Australia and Southeast Asia. However, tinea nigra and the causative fungi may be found worldwide. The fungus is limited to the outermost layer of the skin – stratum corneum. It thrives on the skin of a person who sweats excessively (hyperhidrosis) and is more likely to be making contact with soil and compost.
Tinea Nigra Symptoms
Tinea nigra does not cause an itchy skin rash as is seen with other tinea infections. Most patients are unaware of the fungal infection until the characteristic brown to black rash develops. Although the palms and less commonly the soles are affected, it is possible for tinea nigra to occur on any part of the body. Tinea nigra has an incubation period of between 2 to 7 weeks meaning that the first symptoms may only be present after this period of time has passed since the infection was acquired.
Tinea Nigra Rash
The typical tinea nigra rash does not present with the skin redness (erythema) and a very scaly rash associated with fungal infections. Instead it may appear as :
- Round, oval or irregular shaped flat rash.
- Single solitary lesion although multiple lesions can occur.
- Light brown to dark discoloration depending on a person’s natural pigmentation.
- Clearly demarcated borders separating the discoloration from the unaffected skin.
- Slow growing rash that expands over weeks and months.
- Varies in size from a few millimeters to several centimeters over the long term.
- Mainly on the palms or soles but can also be seen on other parts of the skin, especially on the neck and chest.
Tinea Nigra Pictures
All images have been sourced from the Dermatology Atlas (2) courtesy of Samuel Freire da Silva, M.D.
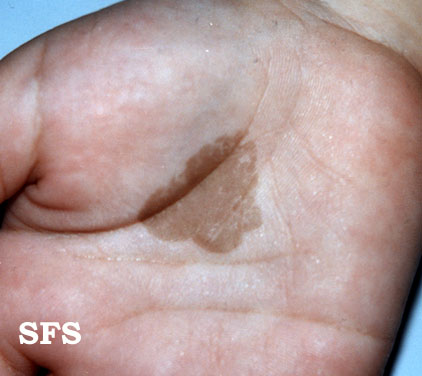
A close up picture of the tinea nigra rash.
Picture of tinea nigra on the palm
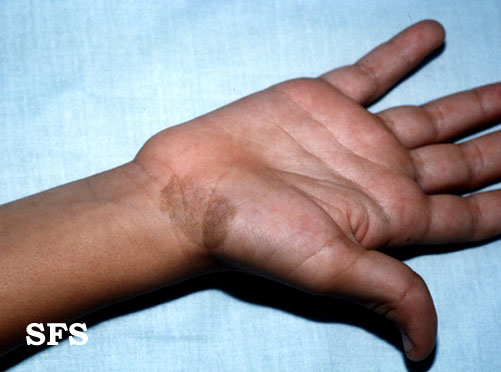
Picture of tinea nigra on the wrist.
Tinea Nigra Diagnosis
The typical rash of tinea nigra may be sufficient to make a diagnosis. Additional investigations will assist in confirming the diagnosis and this includes :
- Microscopic examination of skin scrapings on KOH mount.
- Fungal culture.
It is important to verify that the discoloration is due to tinea nigra and not other conditions that may cause clearly demarcated darks patches on the hands. This type of rash may also be seen in melanoma, moles, hyperpigmentation following severe or chronic skin diseases and staining of the hand with dyes.
Tinea Nigra Treatment
- Tinea nigra can be treated very effectively with topical antifungals.
- Topical antifungals need to be used for 3 to 4 weeks and sometimes longer in chronic cases.
- Scraping the skin with a scalpel blade prior to commencing treatment will help the action of the topical antifungals. This scraping should only be done by a medical professional.
References
1. Tinea nigra. DermNet NZ
2. Tinea nigra pictures. Dermatology Atlas
3. Tinea nigra. Emedicine Medscape