Hair Dye Allergies
What is a hair dye allergy?
About 5% of permanent hair dye users develop an allergy, mostly in the form of an allergic contact dermatitis with a redness and itch in the head area. A systemic reaction with an involvement of the whole body skin and other organs, although rare, is possible in severe cases (1). Understandably dermatitis of the hands affects many hair stylists who are making bare skin contact with these dyes. (2).
The main cause implicated in hair dye allergies, whether on the scalp, face, neck, back or hands, is a substance commonly known as PPD. The most common symptoms is an itchy scalp or burning of the scalp within a short period of time after applying the dye. Sometimes symptoms may develop days or weeks after the hair dye treatment.
PPD (4-ParaPhenyleneDiamine, C6H8N2)
PPD is widely available on the market since 1909, and it is still used in over 2 out of 3 of permanent hair dyes (2007). Commercial hair dye products typically come in two bottles – the one with PPD-based dye (non-oxidized and thus colorless) and the other with oxidizer or developer, usually hydrogen peroxide (H2O2).
In the hair dying process, the peroxide is initially used to break down the natural skin and hair pigment known as melanin. Then the PPD is used to replace the hair color. When PPD reacts with peroxide, it becomes partly oxidized and colored – it is this form that it may cause an allergy.
Fully oxidized PPD does not cause an allergy, so PPD sensitive persons can safely wear fur coats dyed with PPD (3). PPD can be also found in some dark colored cosmetics and temporary tattoos. In France, Germany and Sweden, PPD was banned as a hair dye because it is believed to have serious toxic effects on and in the human body (4).
Alternative names for PPD: PPDA, Orsin, Rodol, Ursol.
PPD and PPD Related Substances
Other hair dye substances that can cause an allergic reaction includes 6-hydroxyindole, Isatin, p-Methylaminophenol (5). Substances related to PPD that may also cause an allergic reaction include :
- Azo groups (chemically: R-N=N-R) used in temporary hair dyes, ballpoint pen inks, gasoline and as coloring agent in foods and medication.
- Local anesthetics benzocaine and procaine.
- Sulfa drugs.
- Para-aminobenzoic acid (PABA) in sun-protective creams.
- Para-aminosalicylic acid used for treatment of tuberculosis.
Hair dyes producers may use misleading terms and users are always advised to discuss this terminology with a hair styling professional or even a doctor in the event of an allergy. “Hypoallergenic” hair dyes are less likely to cause allergies but an allergic reaction is still possible.
“Fragrance free or unscented” only means the product has no odor but this does not necessarily mean that it is devoid of an allergenic properties. A hair dye that is completely “natural” can still trigger an allergic reaction in a sensitive person – it is a matter of individual susceptibility even though majority of the population may not experience any reaction.
Video about Hair Dye Allergies
The following video on hair dye allergies was produced by the Health Hype team.
Types of Allergies Caused by Hair Dyes
Allergic contact dermatitis (ACD) is an immunologic skin reaction occurring in a genetically predisposed individual. The risk of becoming sensitive rises with coloring frequency (6). At least 10 days after initial use of PPD is required for an individual to develop a specific sensitivity. On the second and subsequent exposures to PPD, an allergic reaction can develop within 6 to 72 hours (delayed hypersensitivity).
In this process, the PPD molecules are targeted by certain immune cells (macrophages and lymphocytes) causing the formation of skin granulomas, redness or vesicles. Affected areas – the eyelids, ears, skin at hair line, beard or neck – are usually well demarcated but the irritation may extend beyond the site of contact with a hair dye. Symptoms are itching or burning feeling.
Contact urticaria can develop in minutes to about 1 hour after exposure to a hair dye. PPD triggers the production of IgE antibodies and the release of histamine causing dilatation of the blood vessels in the skin and also makes these vessels more porous.
The increased blood flow along with plasma seeping into the tissue spaces of the skin resulting in skin redness and edema (swelling of the eyelids) . Contact Urticaria Syndrome (CUS) with red patches over the entire body, and bronchial asthma with wheezing, sneezing, difficult swallowing and vomiting can appear.
Anaphylactic shock is an extremely rare but life threatening condition. Facial swelling, gasping for air, drop blood pressure fall and even death can occur if immediate medical attention is not forthcoming.
In an apparent death from anaphylaxis, it was reported that a 38 year mother died in the United Kingdom in August 2000 shortly after changing her hair dye. She was an asthmatic and firstly developed an allergy with a scalp itch after using her old hair dye for some months. After changing the dye, anaphylactic shock developed and she died within an hour after applying the dye. (7, 8)
Allergy Sensitivity Test
Hair dye users can apply a solution (dye and developer mixed together) behind the ear or on the inner side of the elbow for 48 to 72 hours. If there is no irritation (itching / burning) or rash within this time then test is considered negative and the hair dye may be considered as safe to use. If a rash of a certain size (according to a test scale) develops, this is a sign of allergy.
Dermatologists will use a patch test (9). A patch with a 2% PPD in petrolatum is applied to the upper back and examined after 48 hours. Negative reactions show no skin changes; a positive reaction can vary from a mild rash to prominent blistering or even ulcerations. In the “ready-to-use” T.R.U.E. patch test, 24 possible allergenic substances, including PPD, are tested at once (10).
Treatment of PPD Allergy
In an acute severe hair dye dermatitis caused by PPD, the hair and scalp has to be washed thoroughly with a mild shampoo. A solution of 2% hydrogen peroxide or a compresses with potassium permanganate in a 1:5000 dilution is applied to completely oxidize the PPD. To soften the crust, a wet dressing of olive oil and lime may be used. Always speak to your doctor or dermatologist before undertaking these measures.
The patch test has to be conducted afterwards to determine if an allergy to PPD exists, or there is only a non-allergic contact dermatitis present. In the case of a proven allergic dermatitis, a corticosteroid cream which reduces the allergic immune response and therefore inflammation can be applied.
Currently, there are no permanent hair dyes that can be safely used by PPD allergic individuals (2007).
Hair Dye Allergies Related Images
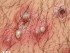
- Allergic contact dermatitis of the neck, caused by hair dye
- Dermatitis behind the ear
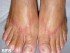
- Allergic contact dermatitis of the hand
Related Articles:
- Types of Skin Rash – Terms Explained
- Scalp Itch – Pictures
- Facial Itch – Pictures
- Itchy Eyelids
- Itchy Neck
- Causes of Itchy Skin
- Itchy Skin – Diagnosis and Treatment
References:
1. Hair dye allergy symptoms (webmd.com)
2. Allergy in hair-dressers (occderm.asn.au)
3. PPD in fur coats (dermnetnz.org)
4. PPD banned (news-medical.net)
5. Hair dye subsatnces causing allergy (ec.europa.eu)
6. Allergic contact dermatitis (emedicine.com)
7. Anaphylactic shock (bbc.co.uk)
8. Skin patch test (dermnetnz.org)