Hernias (Protrusions) Types, Symptoms and Causes
What is a Hernia?
A hernia is an abnormal protrusion of the contents of a cavity through its walls. Hernias are most commonly seen in the abdominal cavity and hence the term hernia is often used synonymously with an abdominal hernia. In this type of hernia, the abdominal contents like parts of the small intestine may protrude through the cavity wall.
Parts of a Hernia
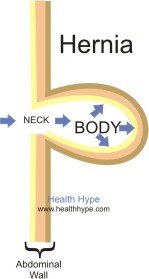
A hernia consists of the hernial sac, its covering (outer part) and contents (inner part). In the abdominal cavity, the hernial sac is a pouch formed out of peritoneum – a thin membrane like covering of the abdominal cavity. The coverings of the hernia include the layers of abdominal wall through which the hernial sac passes through.
A hernia has a neck and a body. The neck of the hernia is the narrowest part of the hernial sac near the orifice or defect in the abdominal wall, while the remaining part of the hernial sac is called the body. The contents of hernial sac vary widely depending on the site of the hernia and size of the hernial orifice. It can include any of the abdominal contents ranging from the small pieces of omentum (peritoneum surrounding organs) to large coils of the intestines.
Types of Hernias
Common types of hernias include :
- Inguinal hernias (indirect or direct) are the most common types of hernias and develop in the groin region.
- Femoral hernia also present near the groin, but slightly lower than and away from inguinal hernias.
- Umbilical hernias are a protrusion through the umbilical scar which are mostly congenital and self limiting.
- Epigastric hernia is a midline hernia in the anterior abdominal wall above the umbilicus.
- Incisional hernias develop in patients with a weakened abdominal wall due to a surgical incision.
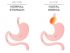
- Hiatal hernia is protrusion of upper part of the stomach into the thorax.
Other less common hernias include an obturator hernia, diaphragmatic hernia, spigelian hernia, lumbar hernia, perineal hernia and sciatic.
Symptoms of a Hernia
The signs and symptoms of a hernia can vary depending on the site and severity of the hernia. Initially a hernia may appear as a painless lump which can be pushed back into the abdomen (reducible hernia). It will however protrude again once the intra-abdominal pressure increases, like during standing or coughing (cough impulse). In these early stages, there may be a dull aching pain but the area is not tender to touch. Although rare, some patients may complain of severe pain at the reducible stage.
As the condition progresses, the hernia may become irreducible or incarcerated. More severe symptoms may be seen at this stage especially in the event of a strangulated hernia. This may include tenderness and swelling at the area. Fever and a malaise may also be reported and in instances of intestinal obstruction, nausea and vomiting may also be seen. A strangulated hernia can lead to complications which could be fatal.
Causes of Hernia
Hernias arise as a result of raised pressure within the cavity and/or weakness of the cavity wall. This can be congenital or acquired. In terms of the abdominal cavity, intra-abdominal pressure is increased in patients with a chronic cough, constipation, urinary retention and ascites (fluid accumulation in abdominal cavity). Weightlifters and any person carrying heavy weights on a regular basis are at high risk of developing hernias. In addition, the abdominal wall may be weakened by obesity, advancing age, multiple pregnancy, surgical incisions or diseases like Marfan syndrome. Presence of some congenital defects (like persistent remnants of processus vaginalis) or weakness in the abdominal wall at birth (like weak umbilical scar) can increase the risk of hernia.
Incisional hernia
Incisional hernias develop after surgical procedures involving the abdominal wall. This post-operative type of hernia occur as a result of inadequate healing of the surgical incision due to wound infection or due to excessive tension at the suture site.
With time an incisional hernia enlarges leading to complications like intestinal obstruction, pain and incarceration. Strangulation is less common as the neck of the hernia is usually large. Risk factors include :
- lifting heavy weights
- malnutrition
- constipation
- persistent cough during the post-operative period
- age
- obesity
- ascites
- pregnancy
Diabetes mellitus (sugar diabetes), corticosteroid therapy, immunosuppressant therapy or wound infection can delay the healing of the incision wound and increase the chances of an incisional hernia developing. Abdominal surgical incisions that damage the nerves that supply the muscles of the abdominal wall also increase the risk of an incisional hernia.
Incisional Hernia Treatment, Surgery (Repair)
Incisional hernias are the most difficult hernias to treat and recurrence is common. Surgical repair of an incisional hernia involves dissection of the hernial sac, reduction of the sac and correction of the defect in the abdominal wall. A mesh is frequently used in repair of the defects in an incisional hernia.
Epigastric Hernia
An epigastric hernia can develop through the linea alba above the umbilicus (navel, belly button). The linea alba is the midline that runs from the xipoid process (bottom of the breastbone) all the way to the pubis.It is often seen in people with well developed abdominal muscles that separates the left and right rectus abdominis muscles.
Epigastric hernias are common in men, especially men who are physically active and doing manual labor. It begins as a small protrusion of extraperitoneal fat through the linea alba. A small peritoneal sac develops and a small piece of omentum may also eventually protrude through. In some patients with larger defects, intestines or other abdominal viscera may get herniated.
Epigastric Hernia Surgery (Repair)
Epigastric hernias are ideally repaired surgically, even if it is small since the herniated extraperitoneal fat is difficult to be reduced in a long standing epigastric hernia. Small epigastric hernias are conventionally repaired under local anesthesia and involve excision of the irreducible fatty tissue and simple closure of the defect. Large epigastric hernias containing herniated omentum or abdominal viscera require reduction and often require a prosthetic mesh for repair.