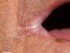
Cheilitis Glandularis (Lip Gland Swelling)
What is cheilitis glandularis?
Cheilitis glandularis is an abnormal enlargement and protrusion of the lower lip with the loss of the clear demarcation between the lip surface and the surrounding skin. The delicate lining of the inner lip becomes exposed to the environment gradually damaging it and sometimes leading to infections. Cheilitis glandularis is rare and poorly understood. It should not be mistaken with other lower lips disorders often caused by biting, excessive licking, sun damage to the lip and abnormal drying of the lip.
The term cheilitis glandularis is used to describe changes in the lip rather than being a diagnosis on its own. The exact reason for these changes is unclear although it is believed to revolve around dysfunction of the minor salivary glands on the lip. Even microscopic examination of the lip tissue may show different changes among patients and the minor salivary glands may be completely normal in some instances. Despite the condition being vague in terms of the underlying disease process, causes and even responsiveness to treatment, it is needs to be attended to as it will continue to worsen over time and even increase the chances of squamous cell carcinoma (cancer) of the lip in some cases.
Picture from Wikimedia Commons
Types of cheilitis glandularis
The term cheilitis refers to the inflammation of the lip and there are various different types of cheilitis which are not necessarily related. Cheilitis glandularis is lip inflammation associated with malfunction of the minor salivary glands. There are broadly three types which are believed to be the mild, moderate and severe stages of the same condition. This includes :
- Simple
- Superficial suppurative
- Deep suppurative
The condition initially starts as simple cheilitis glandularis marked by inflammation of the salivary ducts with swelling of the lip. It can become progressively worse and eventually infected. It then progresses to the superficial suppurative form also known as Baelz diseases. Over time if it is left untreated it can eventually become the deep suppurative form which is also referred to as myxadenitis labialis.
Cheilitis glandularis reasons
The minor salivary glands in the inner lip lining (mucosa) contribute small amounts of mucus in the mouth. It is these glands that appear to be affected in cheilitis glandularis. The glands are inflamed and so are its ducts and surrounding tissue. This is ongoing over long periods of time and some of the ducts may become narrowed leading to accumulation of saliva and formation of retention cysts. Some of the ducts are also abnormally widened allowing for small amounts of thick secretions to constantly leak out.
Cheilitis glandularis causes
The exact cause of cheilitis glandularis is unknown. It is important to note that cheilitis glandularis is a consequence of some underlying disease that causes disturbances in the minor salivary glands. The changes in the lip is a result of exposure to the environment as the swelling causes eversion (turning outwards). Men between the ages of 40 and 70 years seem to be more likely to suffer with cheilitis glandularis. The condition can, however, also occur in women and children.
Genetic factors have been proposed as a possible factor in cheilitis glandularis but this has not been conclusively proven. The condition has also been seen in HIV infected patients and is believed to a manifestation of HIV, although it does not occur in every person infected with the virus. It is as yet unclear whether trauma, tobacco use, infection and prolonged use of antibiotics may be contributing factors to the development of the condition or simply worsen a mild existing case (simple cheilitis glandularis).
There is no significant evidence to suggest that certain mouth diseases like oral thrush (candidiasis) and oral lichen planus more likely to progress to cheilitis glandularis. However, the treatment may be complicated by the presence of these other diseases.
Cheilitis glandularis symptoms
Signs and symptoms of cheilitis glandularis depends on the severity and duration of the condition. It is not uncommon for it to be asymptomatic in the early stages meaning that there are no symptoms. The condition is chronic and progressive and patients may only seek treatment months after it starts. The symptoms include :
- Lip swelling
- Clear thick secretions on the everted lip
- Occasional pustular secretions when infected
- Episodes of lip pain
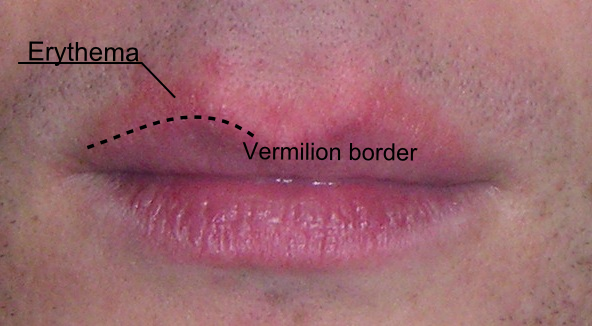
- Burning and rawness of the lip-skin border (vermilion border)
- Shrinking, erosion and ulceration of the vermilion border
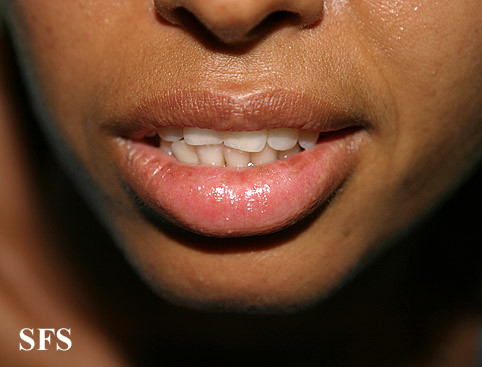
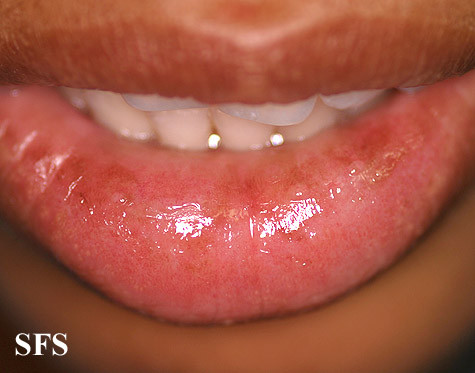
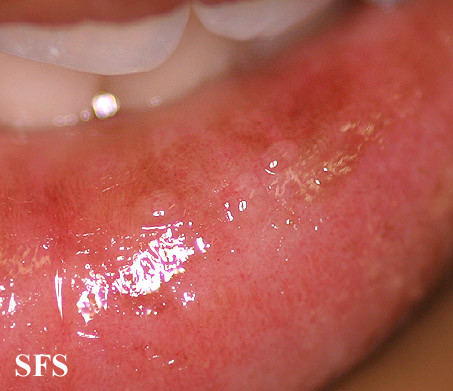
Pictures of cheilitis glandularis
Pictures below from Dermatology Atlas (Brazil) courtesy of Samuel Freire da Silva, M.D.
Cheilitis glandularis diagnosis
Several systemic diseases can cause similar changes in the lip to cheilitis glandularis. This includes sarcoidosis and Crohn’s disease. The latter, Crohn’s disease, is an inflammatory bowel disease but can affect any part of the gut including the mouth and lips. Cheilitis glandularis also needs to be differentiated from angioedema of the lip where there is pronounced swelling and enlargement of the lip often due to an allergic reaction. The following tests may be considered :
- Blood tests
- Bacterial or fungal culture
- Lip biopsy
- Minor salivary gland (lip) biopsy
Cheilitis glandularis complications
People with cheilitis glandularis are are greater risk of squamous cell carcinoma of the lip. This is more likely in Caucasians and the contributing factor in this regard may be sunlight exposure. Bacterial infections are also more likely which is seen with long term untreated cases. The formation of retention cysts and ulcers are not complications as such but part of the disease process. Hyperpigmentation (darkening) may occur in some cases with repeated irritation of the lining.
Cheilitis glandularis treatment
There is no definitive treatment for every case of cheilitis glandularis. Treating any underlying diseases of the mouth or lip should be the first priority even if it appears to be unrelated to cheilitis glandularis. However, since the condition is so uncommon, treatment has to be selected on the individual case. Some of the treatment measures that may be considered includes :
- Antihistamines are prescribed for angioedema but are not effective for cheilitis glandularis on its own.
- Antibiotics may be commenced for bacterial infections and combined with topical immunosuppressants for superficial suppurative forms.
- Topical immunosuppressants and immune modulators may be prescribed for cheilitis glandularis with conditions such as oral lichen planus.
- Surgery may be necessary in some cases and this may include vermilionectomy, cryosurgery or laser surgery.
References :