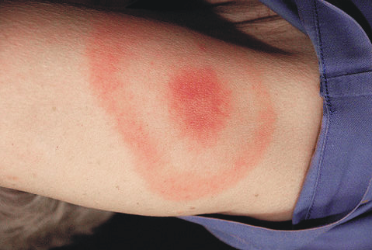
Lyme Disease (Borrelia burgdorferi Bacteria)
What is Lyme disease?
Lyme disease refers to the body’s immune response to the bacterial infection caused by Borrelia burgdorferi. These bacteria are transmitted to humans through bites of the Ixodes ticks. This black-legged tick or deer tick is the main vector of Lyme disease. This tick-borne disease is common in northern part of the United States and in northern California on the west coast.
How common is Lyme disease?
Lyme disease is endemic in northern parts of the USA, Europe, and Asia, where the vectors (ticks) are distributed. The causes of increased incidence of tick disease are expansion of deer herds and the extended range of the vector. I. scapularis species is more common in the Northeast and Central part of United States and Canada, whereas I. pacificus is found on the Pacific coast. I. persulcatus or taiga tick is the principal vector in Asia. The vector in Europe is I. ricinus.
In the United States, this fastest growing vector-borne disease spreads from May to November. 250, 000 cases of Lyme disease were reported between the years 1992 to 2006. Every year, around 20,000 new cases are reported in the United States and Europe. However, the actual incidence of Lyme disease could be much higher than this number.
25% cases of Lyme disease are made up of children younger than 14 years.
Stages of Lyme Disease
The disease progresses in three stages.
Stage 1
In this stage, the bacteria may be present in the body, but the patient may not show any symptom.
Stage 2
In this stage, the bacteria spread throughout the body and produces symptoms. In the early stages of the disease, a skin rash called erythema migrans commonly develops.
Picture of erythema migrans from Wikimedia Commons
Stage 3
In this stage, an immune response to B. burgdorferi infection results in symptoms in various organs.
Location
The bacteria tend to grow in the cells of the skin, central nervous system (CNS), heart, joints, and eyes. The bacteria can also be seen in the bone marrow, testes, the spleen, the liver, lymph nodes, and the placenta.
The lesions formed in the Lyme disease are called borrelial lymphocytomas, which are collection of cells of immune system. Children develop borrelial lymphocytomas on the ears, whereas adults tend to develop lesions on the nipples.
What happens in Lyme disease?
Many of the symptoms of the Lyme disease are caused by active bacterial infection while others result from body’s immune reaction to this infection. Although B. burgdorferi bacteria can affect any part of the body, if they enter the circulation, they have a predilection for certain sites as mentioned above.
B. burgdorferi colonizes in the infected Ixodes ticks, and then transmits to mammalian hosts (like humans). The life cycle of the Ixodes tick has four stages of development: egg, larva, nymph, and adult. The larvae, nymphs, and adult female ticks need blood meals. However, only nymphs and adult ticks can transmit B. burgdorferi.
Method of spread
The Ixodes larvae feed once in the late summer, nymphs feed once on the white-footed mice or other animals in the following spring and summer, and adults feed on the white-tailed deer once in the fall. If these animals are already infected, the Ixodes ticks acquire B. burgdorferi infection. When the infected tick bites a persin, it spreads the infection to humans.
Nymphs are responsible for 90% transmission in humans as they are smaller, present in greater numbers than adults, and because humans are easily available in the summer when nymphs feed.
In the human body
B. burgdorferi live in the mid-gut of the ticks, from where they move to the salivary glands. When an infected Ixodes tick bites a human, the bacteria are introduced in the skin. Once in the skin, the bacteria can meet any of the following fates:
- They may be eliminated by immune mechanisms.
- They may remain viable at the site of introduction or attack the surrounding local tissue.
- They may enter blood circulation and lymph nodes within days or weeks after the initial infection.
Signs and Symptoms
The ticks are very small and the bites are often painless. However, a full-blown infection may present the following symptoms, arranged according to the stages:
Stage 1
- Appearance of erythema migrans (mostly during May – September) in the early stage of the Lyme disease
- Joints affected (in case of B. burgdorferi sensu strict strain)
- Appearance of a characteristic skin rash (acrodermatitis chronica atrophicans), discolored skin, and swelling, in case of infection with B. burgdorferi afzelii strain
- Feverish state
- Itching or burning in erythema migrans
- Expanding rash at the site of the tick bite. If untreated, the rash persists for 2 to 3 weeks
- Flu-like symptoms
- Fatigue
- Discomfort
- Neck stiffness
- Headache
- Joint pain
- Fever
- Chills
Stage 2
- Other organ systems affected
- Neurological symptoms (memory lapses, changes in personality, sleep pattern, and language abilities, concentration, mood swings, depression, and irritability)
- Dizziness
- Fainting
- Breathlessness
- Chest pain
- Palpitations
- Arthritic pain in the knee, ankle, and wrist
- Appearance of borrelial lymphocytoma (bluish-red swollen node) on the earlobe, nipple, nose, and scrotum
Stage 3
- Muscle weakness on one side of the body
- Lack of muscle coordination
- Seizures
- Impairment of cognitive (mental) abilities
- Bladder dysfunction
- Hearing loss
- Discoloration and inflammation of skin of hands, feet, knees, and elbows in elderly
Causes and Risks
Lyme disease is caused by Borrelia burgdorferi bacteria which is transmitted to humans through the Ixodes ticks. Part of the disease is a result of the infection itself and part of it is due to the immune system reaction to the presence of these bacteria in the body.
Living in or traveling to the areas of dense deer population increases the risk of developing the Lyme disease. People who work in the wilderness in these areas are at a greater risk, especially if the are handling deer – veterinarians, hunters or game/wild meat handlers. Domestic pets that travel to high risk regions may carry the tick back with them only to infect humans later on.
Tests and Diagnosis
The following tests can be used to diagnose Lyme disease:
- Antibody detection test can show the exposure to B. burgdorferi bacteria but cannot confirm infection.
- Synovial fluid of the joints can reveal inflammation and is checked to rule out gout.
- Presence of erythema migrans and/or borrelial lymphocytoma helps in diagnosing Lyme disease.
Treatment and Prevention
Treatment aims at curing B. burgdorferi infection, at providing relief from clinical symptoms, and at preventing complications. It is important to note that there is no vaccine to prevent Lyme disease and having it in the past does not mean a person is immune.
Precautions
The best way to prevent Lyme disease is by taking precautions such as :
- Using long sleeved shirts and long pants to protect the skin from tick bites.
- Frequently checking for ticks on pets and children in particular.
- Insect repellent on the skin and clothing can keep the ticks at bay. If a tick is found, it must be removed carefully with tiny forceps (tweezers).
Medication
Antibiotics are given to treat Lyme disease. The choice of antibiotics depends on the patient’s age, allergies, clinical symptoms, stage of disease, and other medical conditions.
- Doxycycline, amoxicillin, or cefuroxime are given for 10 to 14 days to treat Lyme disease. However, doxycycline is not given to young children and pregnant women.
- Pregnant women are not given preventive course and are given antibiotics only after confirm diagnosis of Lyme disease.
- Cefuroxime is given to patients, who are unable to take amoxicillin or doxycycline.
- If the patients present neurological symptoms, penicillin, ceftriaxone, or cefotaxime are given for 2 weeks.
Complications and Prognosis
- If treated in the early stages, Lyme disease can be cured and complications are unusual. Complications may arise in untreated or late stages of Lyme disease and primarily include neurological problems.
- If treated promptly, patients of Lyme disease have a good prognosis. However, patients with undiagnosed and untreated neurological symptoms can suffer from cognitive dysfunction, which can be difficult to treat.
- The prognosis for patients with erythema migrans, who received prompt treatment, is excellent. Similarly, appropriately treated children also have a good prognosis and show complete recovery. In adults too, the long-term outcome is good.
References :