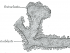
5 Signs of Osteoporosis (Brittle Bone Disease)
Ostoporosis is the most common bone disease that is due to problems with the way bone is removed and replaced. These processes are ongoing throughout life. However, when the degree of bone removal is not matched by bone replenishment, then bones can become weak and brittle. Almost 10 million Americans have osteoporosis and approximately 2 million fractures in the United States are due to osteoporosis.
What Happens In Osteoporosis?
We often tend to think of bones as being massive calcium deposits that complete development by adulthood and remain the same thereafter. This is untrue. Human bone is constantly changing. There are two types of cells responsible for this remodeling activity – osteoblasts that lay down ‘new’ bone and osteoclasts that remove ‘old’ bone. However, only about 1% of the bone deposition and resorption is occurring at any one time.
Nevertheless the other 99% of the bone is being maintained by cells known as osteocytes. In early life the osteoblastic activity (bone deposition) is greater than osteoclastic activity (bone removal). Gradually the osteoblastic and osteoclastic activity become somewhat equal in adulthood. However, this balance is disrupted with advancing age and other factors. Osteoclastic activity exceeds osteoblastic activity which means that more bone is removed than deposited.
Read more on bone formation.
As a result of this shift, the bones become weak and brittle. Initially the bones are not significantly weakened to fracture with ease. A person with early osteoporosis may not experience any greater bone weakness. However, if a fracture does occur then the bone healing is slower than normal. As osteoporosis progresses, then the bones become brittle to the point that even minor injury can cause a fracture.
It may even reach a point where fractures can occur just by the force of the normal body weight. Bone healing is slow and becomes slower as osteoporosis advances. Eventually the ability of the bones to heal can become almost completely compromised. It reaches a point where the bones can never fully heal to restore the same strength and shape that existed prior to the fracture.
Who is at risk of osteoporosis?
Osteporosis is usually seen as a disease of the elderly and particularly elderly women. While osteoporosis is most common among postmenopausal women, it can affect males and younger adults. Similarly, osteoporosis may also affect children and teens and is then referred to as juvenile osteoporosis. However, none of these other groups are considered as high risk as postmenopausal women.
Other risk factors for osteoporosis apart from age includes:
- Family history
- Genetic conditions like cystic fibrosis
- Low calcium intake
- Vitamin D deficiency
- Sedentary lifestyle
- Excessive alcohol consumption
- Cigarette smoking
- Certain drugs like corticosteroids
- Endocrine diseases like hyperparathyroidism
- Digestive conditions like celiac disease
- Cancers like leukemia and multiple myeloma
There are several other factors that can increase the risk of osteoporosis. Many of these risk factors are modifiable which means that it can be changed, minimized or stopped altogether. Other risk factors like genetics are non-modifiable. Individuals with non-modifiable risk factors need to be cautious.
For a more compehensive list of risk factors, refer to the causes of osteoporosis.
How To Spot Osteoporosis
Osteoporosis is difficult to indetify based on the signs and symptoms alone until a facture occurs. In fact osteoporosis can be missed for long periods of time. It is therefore advisable that people at high risk of osteoporosis, especially the elderly and postmenopausal women in particular, undergo routine bone density screening. In the early stages there are often no signs of osteoporosis as the bones are not weak and brittle to a degree where fractures occur with minimal trauma.
Bone Pain
Bone pain is common in the later stages of osteoporosis and usually as a result of fractures. Acute pain typically follows an injury, like a fall. However, even the body weight can cause fractures as may occur in the back. The bone pain is often exacerbated by movement and patients prefer to lie still to minimize the pain.
Fractures often do not heal properly and deformities may eventually arise. Pain in these cases may be ongoing for long periods of time. Some of the commonly affected sites in osteoporosis are the back and hip but any bone may be at risk of easy fratures and subsequent bone pain.
Easy Fractures
The strength of the bones are due to the density of the bones. However, in osteoporosis the bone density decreases to a point where the strength of the bones are significantly compromised. Fractures can occur in even people with healthy strong bones, depending on the degree of trauma (injury).
Since bones are strong, it requires significant force in order for a fracture to occur. With osteoporosis, a fracture occurs much easier. A minor fall or even mild blow can lead to a fracture. As the condition worsens, fractures of the rib can even occur with severe coughing.
Stooping
A stooped posture is more likely to occur in the elderly with prolonged osteoporosis. Repeated fractures and collapse of the verterbrae can cause abnormalities in the curvature of the spine, such as kyphosis or dowager hump. This is where there is forward bending of the spine due to the compression at the front of the vertebrae. As a result a hump is formed in the upper back.
Loss of Height
As osteoporosis progresses there may be a measurable loss of height. It is a result of vertebral fracture compression coupled with the abnormal spine curvature (kyphosis). This loss of height occurs gradually. It is therefore important that the height of an osteoporosis sufferer is recorded and monitored over time. However, the loss of height may not be as significant as is sometimes portrayed. It often averages 2cm to 3cm (approximately 1 inch).
Reduced Body Weight
The bones account for approximately 10% to 15% of the adult body weight. This may vary among individuals and genders.As the bone density decreases, the body weight is impact. Reduction in body weight is gradual and may eventually decline below 19kg/m² (body mass index / BMI). In fact a drop in body weight that is greater than 10% of the body weight should be investigated as it may be due to osteoporosis.