Cystitis (Bladder Infection) Types, Causes and Symptoms
What is cystitis?
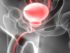
Cystitis is the medical term for inflammation of the urinary bladder. Most cases are due to an infection although other factors such as autoimmune disorders, chemical and mechanical trauma may also cause cystitis. Bacterial infection, often associated with an infection of the urethra (urethritis), is the most common cause of cystitis. Both these conditions are broadly referred to as a urinary tract infection (UTI).
Cystitis is more frequently seen in women because of a shorter urethra and lack of bactericidal prostatic fluid. It can be acute or chronic. Acute cystitis tends to present with more severe symptoms and some cases of cystitis, especially the chronic cases, may be asymptomatic for periods of time.
Urine is generally sterile but provides the ideal medium for bacteria. Most infections ascend up the urinary tract from the urethra to the urinary bladder. It is frequently associated with sexual intercourse due to urethral trauma although it is not a sexually transmitted disease (most are not). Cysitis may also arise secondary to an underlying urogenital condition like benign prostatic hyperplasia (BPH) in men and bladder stones in both genders.
There are three cardinal features of cystitis includes frequent urination, pelvic pain (sometimes reported as abdominal pain) and burning or pain upon urination. A fever and pus in the urine which presents as cloudy urine is more likely to be due to an infection.
Types of Cystitis
There are several different types of cystitis which may be broadly categorized as bacterial or non-bacterial cystitis. The latter, non-bacterial cystitis, comprises a number of causes including other infections (fungi, parasites and viruses) and non-infectious causes. Mechanical trauma as is seen with long term catheterization may lead to bacterial cystitis or inflammation in the absence of an infection.
- Infectious cystitis
- Arises as a result of an infection, mainly bacteria.
- Chemical cystitis
- Associated with hypersensitivity to certain chemicals like soap, bubble bath and spermicidal gel.
- Drug-induced cystitis may be seen in patients use chemotherapeutic drugs.
- Radiation cystitis
- Arises as a result of radiation therapy often in the treatment of pelvic tumors.
- Tuberculous cystitis
- Follows renal tuberculosis.
- Interstitial cystitis
- A chronic bladder inflammation where the cause and pathophysiology is unclear.
How do bacteria enter the bladder?
Microorganisms more frequently reach the urinary bladder through the urethra (ascending infection). Less commonly, these pathogens may travel via the blood stream, direct infiltration from other surrounding structures that are not part of the urinary tract, like the vagina in women or rectum or it passes to the bladder through the lymphatic system.
Urine in most parts of the urinary tract is sterile. Most cases of bacterial cystitis are due to bacteria found in the rectum. When bacteria enter through the distal urethra, it is usually passed out during urination. Coupled with the immune defenses, an infection rarely occurs without other predisposing factors.
Risk Factors for a Bladder Infection
In women, urinary tract infections (often involving the bladder) are common due to a shorter urethra. With men, a bladder infection is less likely to occur because of a longer urethra and bactericidal prostatic fluids unless there is underlying condition like benign prostatic hyperplasia, following kidney or bladder stones or other causes of bladder neck obstruction.
There are other factors that may also be responsible for an ascending infection of the urinary tract. Some susceptible individuals have certain receptors present on the endothelial lining of the urethra to which certain strains of bacteria can attach to. This prevents it from being ‘washed out’ during urination and facilitates the infectious process. Sexual intercourse often leads to minute tears on the urethra that compromises the integrity of this part of the urinary tract.
Many fungal and viral cases may be seen in immunocompromised patients, as is seen with HIV infection or long standing uncontrolled diabetes mellitus (sugar diabetes), and sexually transmitted infections. Candida and other fungal urinary tract infections may also be a result of long term antibiotic use.
Bladder infections may arise without any of the multitude of predisposing factors being present but this is more likely to occur in acute infectious cystitis. Chronic infectious cases are almost always associated with underlying genitourinary pathology.
Other risk factors include :
- Pregnancy
- Inadequate personal hygiene
- Dehydration
- Diaphragm for birth control
Causes of Bladder Infection
There are a number of microorganisms that may cause a bladder infection. Some of the organisms include :
Bacteria
- Escherichia coli
- Proteus mirabilis
- Streptococcus fecalis
- Staphylococcus saprophyticus
- Klebsiella spp
- Chlamydia trachomatis
- Mycobacterium tuberculosis
Virus
- Herpes simplex (HSV-1 and HSV-2)
- Adenoviruses
Fungus
- Candida albicans
- Cryptococcal spp
Parasites
- Schistosoma haematobium
Symptoms of Bladder Infection
The three cardinal symptoms (triad) of bladder inflammation, including infectious cystitis, include :
- Frequent urination, often waking at night to urinate (nocturia)
- Burning sensation or pain upon urination (dysuria)
- Pelvic pain
Other signs and symptoms of a bladder infection may vary in severity and may be absent at times. This includes :
- Blood in urine (hematuria)
- Cloudy urine
- Strong smelling urine
- Abdominal, flank and/or back pain
- Fever with/without chills
- Nausea or vomiting
Patients may also report pain during intercourse (dyspareunia) which could also be a symptom of underlying genitourinary pathology.