Cardiac Tamponade (Fluid Pressing on the Heart)
What is a cardiac tamponade?
Cardiac tamponade is a condition where the accumulation of fluid around the heart hampers its filling and circulation of blood. The fluid that collects around the heart can either be blood, serous tissue fluid, pus or lymph with fat droplets. Sometimes a solid mass or even gas can restrict the heart movement but these instances are uncommon. The restriction of the heart in a cardiac tamponade means that insufficient blood fills the heart and is subsequently pushed out of the heart to the rest of the body. Therefore there is less oxygen in the circulation. A cardiac tamponade needs emergency treatment and the fluid has to be drained out of the heart. It can be fatal if left untreated.
Why does fluid compress the heart?
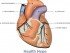
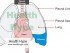
The heart is surrounded by the pericardial sac. It is made up of two layers of pericardium – a visceral pericardium that adheres to the heart wall and a parietal pericardium that overlies the heart somewhat loosely. Between these two layers is the pericardial space. It is filled with pericardial fluid which acts as a lubricant. There is anywhere between 20mL to 50mL of pericardial fluid in the pericardial space which is well accommodated but does not hamper heart expansion during filling.
Fluid accumulates around the heart
Fluid accumulation around the heart in the pericardial space is called a pericardial effusion. Mild effusions may not cause any significant disruption of heart function. However, significant collection of fluid in the pericardial space acts as physical barrier by applying pressure from outside the heart.
The heart enlarges when its muscles relax and the heart fills with blood. The filling has to be adequate in order for sufficient blood to be pumped out of the heart during systole (contraction of the ventricles). With a pericardial effusion, the accumulated fluid does not allow for the ventricles to fill to its full capacity.
The heart cannot contract properly
The strength of the ventricular contraction is also dependent on the degree of filling (volume). The greater the volume of blood filling, the more the heart wall stretches due to the pressure within the ventricle. Therefore the greater the force with which it will push out blood. However, expansion of the heart and the volume of blood that can fill the relaxed ventricle is hampered by the effusion. This is known as a cardiac tamponade.
Both the volume of blood and the force with which it is pushed out is diminished with a cardiac tamponade.
What are the symptoms of a cardiac tamponade?
A cardiac tamponade is a medical emergency. However, the symptoms may not always be intense at the outset.
Lower Heart Output
The symptoms of a cardiac tamponade are mainly due to less blood leaving the heart and therefore the body’s tissues receiving less oxygen. These symptoms includes :
- Shortness of breath (dyspnea)
- Rapid breathing (tachypnea)
- Rapid heart rate (tachycardia)
- Anxiety
- Dizziness
Very low blood pressure, paleness or bluish discoloration of the skin, fainting and a weak pulse are signs of shock. It is a result of inadequate blood circulation throughout the body.
Chest Pain
Chest discomfort is present to some degree in most cases but pain is not always present. When chest pain does occur, it is at times mistaken for heart attack pain. However, chest pain in a cardiac tamponade does differ in various respects to heart attack pain. It has the following characteristics :
- Sharp stabbing pain (cardiac tamponade) compared to crushing, squeezing and tight chest pain (heart attack).
- Pain radiating to the shoulder, back or abdomen compared to heart attack pain which radiates to the jaw and arm.
- Pain worsened with deep breathing and coughing.
- Pain eases with sitting upright or leaning forward.
What causes a cardiac tamponade?
A cardiac tamponade is result of a pleural effusion – fluid collection around the heart. Very rarely is gas responsible for this compression. Even though a solid mass, like a tumor, can press against the heart it does not often impair ventricular filling to the same degree as fluids. In fact, a tumor may instead irritate the pericardial lining and cause it to secrete more fluid or block lymph drainage which are the causes of the cardiac tamponade.
- Pericarditis (inflamed pericardium) due to :
– Infections – viral or bacterial more common.
– Chest injury.
– Drugs.
– Radiation therapy.
– After a heart attack (myocardial infarction).
– Following chest and heart surgery.
– Autoimmune diseases.
– Idiopathic (unknown causes). - Cardiac and pericardial tumors.
- Thoracic aortic aneurysm (dissection).
- Uremia.
- Anticoagulant therapy.
The fluid in a cardiac tamponade may be from the pericardium, heart or blood vessels.
- Hemorrhagic – blood
- Chylous – fat and lymph
- Serous – thin watery usually clear fluid
- Serosanguinous – combination of serous fluid and blood
How is cardiac tamponade diagnosed?
The symptoms alone are not conclusively indicative of a cardiac tamponade. During a clinical examination, a doctor may find certain signs that raise the suspicion of cardiach tamponade :
- Faint heart sounds – heart beats may sound soft or muffled.
- Pericardial friction rub – an extra heart sound that is grating or squeaky in nature.
- Pulsus paradoxus – fall in blood pressure during deep inspiration (inhalation).
- Pulses of the hand and legs may be weak or absent.
- Increased jugular venous pressure (JVP) – abnormal distension of the neck veins even with low blood pressure.
Tests and Scans
- Various blood tests may be conducted to confirm the cause of a cardiac tamponade but is not useful for confirming the presence of the tamponade.
- Echocardiography is one of the preferred methods for diagnosing a tamponade. It uses ultrasound waves to create images of the heart action.
- X-ray, computed tomography (CT) scan and magnetic resonance imaging (MRI) of the chest.
- Electrocardiogram (ECG).
What is the treatment for a cardiac tamponade?
A cardiac tamponade requires emergency medical intervention. Supportive measures, medication and surgical procedures are necessary to treat cardiac tamponade.
- Oxygen therapy to improve blood oxygenation and oxygen distribution throughout the body.
- Intravenous fluids, blood or plasma to increase the blood volume and raise the cardiac output.
- Medication known as inotropic drugs increase the force of the heart contraction and therefore the cardiac output.
- Elevating the legs to increase the amount of blood returned to the heart also assists with cardiac output.
These measures are helpful in stabilizing and managing the patient until more invasive procedures can be undertaken.
- Pericardiocentesis is a procedure where a fine needle is inserted into the pericardial sac and the fluid is drawn out. A catheter may be left in place to prevent repeated fluid accumulation.
- Pericardiectomy is a surgical procedure where a portion of the pericardium is removed. It may not be needed in every case of a cardiac tamponade.
The underlying cause of a cardiac tamponade needs to be identified and treated or the condition will very possibly recur.
References