Colon vs Large Intestine – Parts, Symptoms and Diseases
The intestines are the longest part of the digestive tract, running frome the end of the stomach to the anus. There is the small intestine, which is the longest of the intestines, and the large intestines. As the name suggests the large intestine is wider and larger than the small intestine, although shorter.
Parts of the Large Intestine
The large intestine has two distinct parts:
- Cecum where the small intestine joins the large intestine and includes the vermiform appendix.
- Colon which constitutes the majority of the large intestine.
The end portions of the digestive tract, namely the rectum and anal canal, are sometimes considered as a separate part of the digestive tract. However, it is now becoming more popular to include the rectum and anal canal (anorectum) as part of the large intestine.
Parts of the Colon
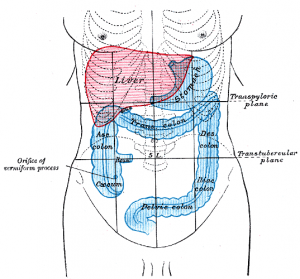
As mentioned, the colon is only one part of the large intestine. The colon itself can be divided into four parts based on its location and orientation:
- Ascending colon is the first part of the colon leading from the cecum. It runs upwards on the right side of the abdomen.
- Transverse colon is the second part extending from the hepatic flexure. It runs across the upper abdomen from the right to the left.
- Descending colon is the third part of the colon extending from the splenic flexure. It runs downwards on the left side of the abdomen.
- Sigmoid colon is the last part and narrowest part of the colon that extends from the end of the descending colon to eventually become the rectum.
Signs and Symptoms
The signs and symptoms of the various diseases involving the large intestine are largely the same and can be difficult to differentiate. These symptoms include:
- Abdominal pain, cramps or discomfort
- Abdominal distension (enlargement)
- Alterations in bowel habit – constipation or diarrhea
- Blood and/or mucus in the stool or from the rectum
- Bloated sensation – feeling of fullness
- Excessive flatulence
- Abnormal bowel sounds – borborygmi
Other symptoms like nausea, vomiting and fever are non-specific and may only arise in certain large intestine diseases. For example. fever may be a sign of an infection.
Read more on colon pain.
Diseases of the Large Intestine
The following diseases may involve the cecum and/or colon. Diseases and disorders of the rectum or anal canal are not included.
Appendicitis
Appendicitis is inflammation of the vermiform appendix. The appendix (vermiform appendix) is the small narrow outpouching from the cecum. It arises when the opening of the appendix becomes obstructed. Bacteria may then multiply within the appendix and cause an infection. In severe cases where treatment is delayed, the appendix can burst which is a medical emergency.
Colorectal cancer
Colorectal cancer is one of the most common types of cancers globally. It arises when cells in the colon or rectum become abnormal and start multiplying rapidly. These malignant (cancerous) growths damage healthy tissue and can spread to other parts of the body. Sometimes cancerous cells from elsewhere in the body can spread to the colon and rectum where it causes cancer.
Colitis
Colitis is a broad term for inflammation of the colon due to a host of different causes. One of the common reasons for colitis is an infection caused by viruses, bacteria and/or protozoa. Sometimes the toxins of these infectious agents or other toxic substances can also cause colon inflammation. A range of other insults such as autoimmune, environmental and circulatory disturbances can also cause colon inflammation.
Read more on types of colitis.
Diverticulitis
Diverticula are abnormal pouches that form in the wall of the colon. These pouches may not cause any signs or symptoms until it becomes infected. The infection of these pouches is known as diverticulitis. Diverticulosis (formation of diverticula) and diverticulitis is more common in older people and particularly among smokers, people who are overweight or obese, live a sedentary lifestyle and consume a low fiber diet.
Inflammatory bowel disease
Inflammatory bowel disease (IBD) is a disorder where the immune system attacks the wall of the digestive tract, particularly that of the bowels (intestines). This causes inflammation and even the formation of open sores (ulcers) with a disruption of normal bowel activity. Of the two types of IBD, ulcerative colitis is limited to the colon whereas Crohn’s disease can affect part of the digestive tract, even without any large intestine involvement.
Irritable bowel syndrome
Irritable bowel syndrome (IBS) is not conclusively linked to the bowels (intestines) alone. The exact cause is unclear and several mechanisms have been proposed. There is no clearly identifiable pathology (disease process) that can be isolated in IBS. It appears to be due to abnormally rapid or slow movement through the bowels. This gives rise to abdominal pain and alterations in bowel habit (constipation, diarrhea or a combination of both).
Ischemic colitis
Ischemic colitis is one type of colitis (colon inflammation) which occurs when the blood flow to the colon is reduced. This leads to insufficient oxygen supply to the colon tissue. It arises when the blood vessels become narrowed or even blocked. Ischemic colitis is more likely to occur in older people, after abdominal surgery and in people who are at risk of atherosclerosis (fatty plaques developing in the artery walls).
Megacolon
Megacolon is an abnormal widening (dilatation) of the colon. It arises when there is weakening, paralysis or dysfunction of the muscles in the colon. This results in the backing up of the contents of the colon and stretching of the colon wall. Megacolon can be acute or chronic. In terms of the latter, the dilatation may be present from birth (congenital), develop in life (acquired) or occur for unknown reasons (idiopathic).
Polyps
Colonic polyps are outgrowths that protrude from the colon wall. Most of these growths are benign (non-cancerous) but some polyps have the potential to become malignant (cancerous). Polyps may not cause any symptoms unless it becomes large or there are multiple polyps in a small area of the colon.
Polyps are a result of disturbances in the genes that control cell growth. Certain risk factors increase the likelihood of colon polps, such as being over the age of 50 years, consuming alcohol and tobacco, a family history of colon polyps and having conditions like type 2 diabetes and inflammatory bowel disease (IBD).