Fluid Around the Lungs (Pleural Effusion) Causes, Symptoms, Drainage
What is a Pleural Effusion?
Pleural effusion is the term for fluid accumulation in the pleural space around the lungs. It is commonly referred to as fluid around the lungs or water surrounding the lungs. It must be differentiated from pulmonary edema which is commonly known as water or fluid in the lungs. The pleural cavity is a potential space between the parietal pleura that lines the inside of the chest wall and the visceral pleura that lines the outer part of the lung.
There is a small amount of fluid in this space (pleural fluid) which serves as a lubricant. It ensures that the two pleural layers do not rub against each other when the lung expands and contracts during breathing. Normally there is about 15 ml of serous fluid in the pleural space. This pleural fluid is clear and similar to interstitial fluid. The pleura do not have secretory cells that produce and secrete mucus as is seen in other cavities.

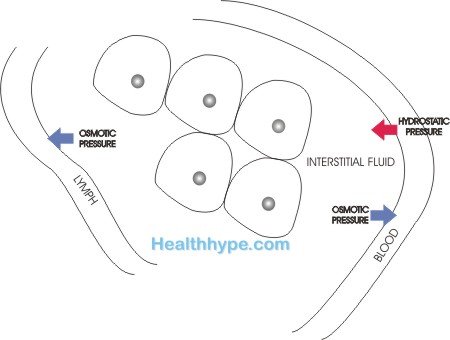
Instead the pleura are serous membranes which allow small amounts of interstitial fluid (tissue fluid) transude continuously into the pleural space. The presence of small tissue proteins gives the fluid a slight mucoid texture. The pleural fluid is constantly taken up by the lympathic vessels to prevent any buildup in the pleural space. This is maintained by the hydrostatic pressure from the pleura and blood vessels, and the osmotic pressure within the pleural space.
Types of Pleural Effusion
Accumulation of fluid around the lungs is similar to edema in any part of the body and a pleural effusion is essentially edema of the pleural cavity. This is explained further under pathophysiology of edema.
As with edema elsewhere in the body, an effusion may occur through one or more of the following mechanisms.
- Increased hydrostatic pressure in the vessels which causes excess fluid to be pushed out into the pleural space.
- Decreased osmotic pressure in the vessels which allows fluid to pass into the pleural space.
- Increased vascular permeability when there is blood vessel damage thereby allowing fluid to leak into the pleural space.
- Raised negative pressure within the pleural space which draws fluid into the pleural space.
- Reduced lymphatic drainage of pleural fluid often due to a blockage of the lymphatic vessel or surrounding lymph nodes.
The pleural effusion may be of two types :
- Transudate when the fluid leaks or is pushed into the pleural space as is seen with increased hydrostatic pressure or decreased osmotic pressure (transudative effusion).
- Exudate when the vascular permeability is increased due to damage or the lymphatic drainage of fluid is impaired (exudative effusion).
Causes of Pleural Effusions
Transudative Effusions
Transudates are indicative of a disturbance in the balance between hydrostatic and osmotic pressure and there is usually no inflammation of the pleura or injury of the pleural capillaries. It is a serous fluid that is similar in composition to normal pleural fluid but excessive. This can be unilateral or bilateral and is known as a hydrothorax.
Causes of transudative exudates includes :
- Congestive heart failure
- Liver failure
- Cirrhosis
- Kidney failure
- Nephrotic syndrome
- Pulmonary infarction (usually a hemorrhagic exudate)
Exudative Effusions
Exudates may be due to inflammation of the pleura or surrounding tissue and injury to the microvasculature and is often a feature of inflammatory conditions. The exudate can be serous, serofibrinous or fibrinous. A serous exudate is similar to the normal pleural fluid with minimal inflammatory infiltrate like lymphocytes. The fibrinous exudate is when the microvascular permeability is increased significantly and fibrin enters the tissue spaces. This can lead to organization and adhesions.
Causes of a exudate, usually without blood or pus, includes :
- Systemic lupus erythematosus (SLE)
- Rheumatoid disease
- Tuberculosis
- Acute pancreatitis (may also be blood-stained)
Different Types of Pleural Exudates
Puruluent exudate is pus in the pleural exudate which is known as an empyema. It occurs with infections in the pleural space, most frequently with bacteria but may also be seen with fungal infections. The pathogenic microorganisms usually spread to the pleural space from surrounding sites, particularly the lung or bronchi or it may reach the pleural space through the blood stream or lympatic system (dissemination). Purulent exudate is yellow to green in color, creamy compared to the normal thin serous fluid with a number of inflammatory cells – neutrophils and other leukocytes.
Causes of purulent exudate includes :
- Infectious pleuritis – pyogenic bacteria, fungi
- Pneumonia
- Intra-abdominal / subdiaphragmatic or abscess, especially liver abscess
Hemorrhagic exudate is the presence of blood in the pleural exudate. It is not a true hemothorax where only blood fills the pleural space as is seen in chest trauma. A hemorrhagic exudate, however, may be just as serious. It is associated with severe vascular damage as blood cells are able to leak out into pleural exudate. This may be microscopic and not visible to the naked eye or can stain the exudate pink, red or darker shades with red blood cell breakdown.
Causes of hemorrhagic exudate includes :
- Pulmonary infarction
- Pulmonary embolism
- Malignancy – cancer of pleura, lung, bronchi, chest wall
- Acute pancreatitis
Chylothorax is the term for accumulation of chyle, a milky fluid high in fats, in in the pleural space. It is seen with lymphatic obstruction where the drainage of pleural fluid via the lymphatic system is compromised. A chylothorax can also occur when there is a rupture of lymphatic vessels.
Causes of a chylothorax includes :
- Thoracic duct obstruction
- Malignancy – pleura, mediastinal carcinomatosis
- Lymphangitis
Symptoms of Pleural Effusion
A build up of fluid in the pleural space can restrict lung expansion. This may manifest as shortness of breath and the severity may vary depending on the extent of the effusion. Rapid shallow breathing may be clearly detectable.
Other signs and symptoms may be associated with irritation of the pleura and not just a result of the effusion. This includes :
- Pleuritic pain – chest pain which is worse on breathing deeply and coughing
- Pleural frictional rub
- Dry cough
Other symptoms, like a fever, may be seen in infectious causes and unintentional weight loss should raise the concern about conditions like pleural tumors.
Diagnosis of a Pleural Effusion
Signs of a Pleural Effusion
A pleural effusion is detectable clinically only when the quantity of accumulated fluid exceeds 500 ml. The following signs may be evident :
- Chest movement in relation to breathing is reduced on the affected side.
- Breath sounds are reduced on the affected side.
- Percussion over the fluid-filled area gives a dull note (stony dullness).
- Tracheal deviation may be a result of the lungs being pushed opposite to the affected side as a result of a massive effusion.
X-ray, Ultrasound and CT Scan
Radiological investigation is the most useful test for detecting the presence of pleural effusion. A minimum of 300 ml of fluid accumulation is required for producing a significant radiological finding (blunting of costophrenic angle) on a regular chest x-ray (posterioanterior view). Effusions as small as 150 ml can be seen on a chest x-ray taken in special views (lateral decubitus view).
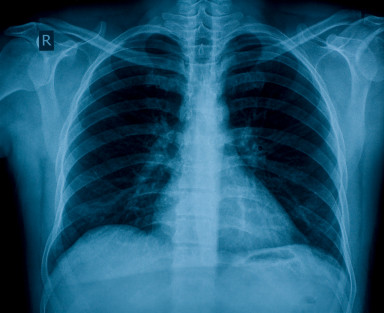
Picture of Normal Chest X-Ray (Posterioanterior View)
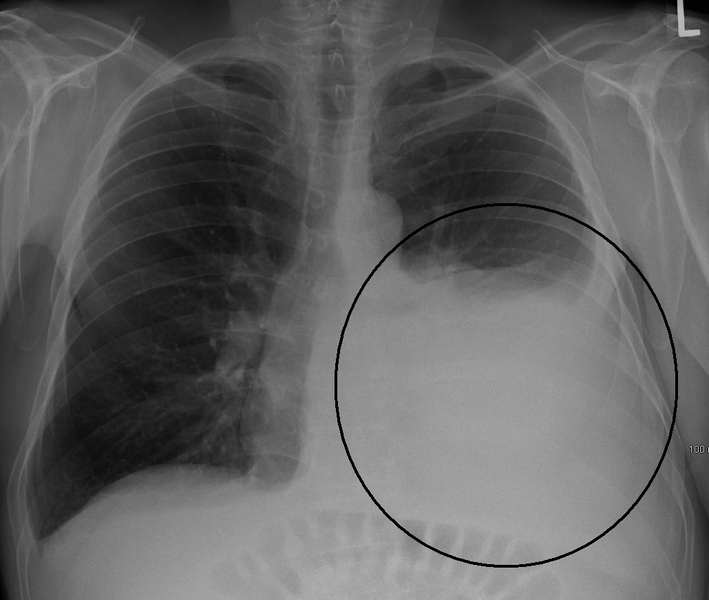
Picture of Chest X-Ray with a Pleural Effusion (Source : Wikimedia Commons)
An ultrasound and CT scan may provide more detailed and accurate information about the pleural effusion. These investigations can also highlight other abnormalities that may be present in the lungs and pleura. Radiological investigations can also differentiate pneumothorax (accumulation of air in pleural cavity) and hydropneumothorax (accumulation of air and fluid in pleural cavity) from a pleural effusion.
Pleural Tap, Biopsy and Exploration
Certain invasive diagnostic procedures are usually performed to determine the cause of the pleural effusion. Pleural tap (thoracentesis) is most important invasive diagnostic procedure performed in individuals with pleural effusion. Other invasive procedures include pleural biopsy and pleural exploration.
Treatment of a Pleural Effusion
The management of a pleural effusion depends on the cause. It is possible for a pleural effusion to resolve spontaneously in some patients. Excessive fluid may be drained for symptomatic improvement along with the measures adopted for the treatment of the cause. In patients with milder effusions, an extended pleural fluid aspiration (therapeutic thoracocentesis) following the diagnostic pleural tap is usually sufficient. Therapeutic thoracentesis involving removal of larger amounts of fluid may require insertion of a tube drain. More than 1 to 1.5 liter pleural fluid should not be removed at a time as it can lead to pulmonary edema (fluid in the lungs). Read more on drainage of pleural fluid.
Recurrent Pleural Effusions
Recurrent pleural effusions causing significant respiratory difficulty are treated more aggressively. Repeated pleural tap may be carried out in such cases. If the effusion is not satisfactorily controlled with pleural taps, tube drainage or thoracoscopic drainage is done. It may be combined with chemical pleurodesis. The effusion is drained as complete as possible. The chemical pleurodesis may be done if the effusion drained per day falls to 150 ml.
Chemical Pleurodesis
Chemical pleurodesis involves scarring the two opposing layers of pleura with chemicals like talc, doxycycline or bleomycin. The chemicals are instilled through the chest tube or following the thoracoscopic drainage. The procedure results in formation of adhesions which prevents accumulation of fluid between the two layers.
Failure of pleurodesis to yield the desired resulst can be managed with placement of chest tube with one-way valve. Drainage with this can be done daily and can be managed from home. Highly refractory pleural effusions may require mechanical pleurodesis (scarring the pleura mechanically during surgery) or pleurectomy.
Treating an effusion in different diseases
Majority of the transudative effusions improve with the correction of the underlying disease like heart failure, nephritic syndrome and so on.
Effusions resulting from lung infections, like pneumonia or a lung abscess, can resolve spontaneously with antibiotic therapy or sometimes may require drainage. Complicated effusions with pus in the pleural cavity (empyema) require immediate drainage and aggressive empirical antibiotic therapy. It is usually drained with a chest tube.
Tuberculous pleural effusions are usually mild and resolve within few weeks of initiation of anti-tubercular treatment. A short course of corticosteroids may be needed in seriously ill patients. Surgical drainage is rarely required in tuberculous effusions.
Effusion resulting from rupture of esophagus is treated with immediate surgical closure of the esophagus. A delayed surgical closure should be supported with antibiotic coverage against anaerobic bacteria, and pleural drainage.
Pleural effusion associated with immunological disorders like rheumatoid arthritis or lupus may resolve spontaneously in some patients. Some patients require short course of steroid therapy for resolution of effusion.
A pleural effusion resulting from malignancy is best managed with a combined approach. The approach involves the treatment of malignancy and treatment of the effusion. The effusion is managed with thoracocentesis, chest tube insertion, or VATS drainage. Recurrent effusions resulting from malignancy may be treated with permanent pleural drainage catheter, pleurodesis (chemical or mechanical) or open surgical pleurectomy.
Drainage of Pleural Effusion
Pleural Tap
A pleural tap can be performed for diagnostic purpose or for therapeutic reasons to drain the fluid around the lungs. A needle or a canula is passed into the pleural space and a small quantity, about 30 to 50 ml, of the fluid is collected for analysis. In some patients, with a small pleural effusion, this diagnostic procedure is usually combined with the treatment. A pleural tap helps in the diagnosis of the cause of the pleural effusion in about 80% of the patients. It may help in excluding certain diseases in the remaining individuals, even if the procedure may not be diagnostic.
The procedure is not indicated in individuals with coagulation (blood clotting) disorders that cannot be controlled. It is also done with great deal of caution in patients on mechanical ventilation as in with emphysema, those with only one functional lung and other high risk conditions.
A pleural tap can be complicated at times by pneumothorax (air accumulation in pleural cavity) or hemorrhage. These complications can be minimized with use of ultrasound for guiding the needle used for the pleural tap. Some individuals can develop sudden hypotension during the procedure (vasovagal). Other complications include pain, surgical emphysema (accumulation of air in the skin and subcutaneous tissue), infection, and puncture of spleen or liver.
Percutaneous Pleural Biopsy
Patients with exudative effusion who remain undiagnosed after pleural tap may require a pleural biopsy for further evaluation. Patients having pleural fluid with a lymphocytic predominance may also benefit from a pleural biopsy. Most frequent diagnosis in these patients is cancer or tuberculosis.
Thoracoscopy
Thoracoscopy may be performed in patients with undiagnosed pleural effusion. Pleural biopsy may be performed under direct visualization through thoracoscopy.
Tests and Results
A wide variety of tests are done with the pleural fluid to find the cause of the pleural effusion. Pleural fluid is grouped as exudative and transudative effusion, based on the protein content of pleural fluid and its lactate dehydrogenase (LDH) concentration.
- In transudative effusion the ratio of total pleural fluid protein to serum total protein is less than 0.5 and ratio of LDH in pleural fluid to serum is less than 0.6. Transudative effusion is suggestive of an imbalance in the fluid balance in the pleural space (example heart failure or liver failure). Usually present on both sides.
- Exudative effusion results from the damage or disruption to pleural integrity or its lymphatic drainage (eg lung infections or malignancy). More often present on one side.
- The pH of the fluid is less that 7.2 in conditions like empyema (pus around the lungs), rheumatoid or tuberculous pleuritis.
- The glucose level of the pleural fluid is also tested and may be found to be low in patients with effusion due to conditions like rheumatoid disease or infections.
- Pleural fluid amylase levels are elevated in patients in whom pancreatic disease or esophageal rupture is the cause for the effusion.
Color of Effusion
- Transudative effusion is usually clear while exudative effusion is cloudy.
- Blood stained pleural fluid may be seen in malignancy and trauma. Presence of red blood cells is a confirmatory sign of hemorrhage. In frank bleeding, the fluid is dark or red colored (hemothorax).
- Pale effusion is seen commonly in patients with generalized edematous conditions like heart failure.
- Milky effusion may be due to a chylothorax.
Cell Count and Cytology
A cell count and cytology can be performed on the pleural fluid. Increase in number of white blood cells is suggestive of infection. A sample with predominant neutrophils is suggestive of bacterial infection and those with lymphocyte predominance may be of tuberculosis or lymphoma. Culture of the pleural fluid is also done to identify the organism and to find the antibiotic sensitivity.
Cytology is important in diagnosis of malignant conditions that can cause effusion. Cancerous cells can be found in the pleural fluid in lung cancer, malignant mesothelioma and metastatic cancer lesions from other sites. Presence of cancer cells in pleural fluid is diagnostic of cancer but their absence does not rule out cancer.
Fats in the Fluid
The cholesterol and triglyceride levels of the pleural fluid are elevated in individuals with leakage of lymph vessels into pleural cavity (chylothorax). Chylothorax is often seen in patients with rupture of thoracic duct due to trauma or cancer. The pleural fluid in these patients usually has a milky appearance.
References
- Pleural Effusion. Medscape
- Pleural Effusion. Merck