Ovarian Hyperstimulation Syndrome (OHSS)
What is ovarian hyperstimulation syndrome?
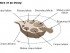
Ovarian hyperstimulation syndrome (OHSS) is an iatrogenic complication, which means it results from treatment-based stimulation of ovaries. This rare condition develops in women undergoing infertility treatments. OHSS may occur after gonadotropin therapy, which is a common type of treatment for infertility. The therapy may lead to the development of ovarian hyperstimulation syndrome approximately 1 to 2 weeks after assisted ovulation or egg retrieval. Ovarian hyper-stimulation syndrome is marked by presence of multiple ovarian cysts leading to enlargement of ovaries. This is in keeping with overactivity of the ovaries but in OHSS it is a result of the treatment.
How common is ovarian hyperstimulation syndrome?
The incidence of ovarian hyper-stimulation syndrome depends on many factors including stimulation methods, risk factors, and conception. Mild OHSS is seen in more than 20% women undergoing ovarian stimulation. Around 7% women are at risk of developing moderate ovarian hyper-stimulation syndrome, whereas less than 5% females develop severe OHSS.
Types of OHSS
Ovarian hyper-stimulation syndrome is divided into following types, depending on the severity.
Mild
Mild OHSS, is further sub-divided into following grades:
- Grade 1, characterized by discomfort and abdominal distention
- Grade 2, characterized by discomfort, abdominal distention, nausea, vomiting, diarrhea, enlarged ovaries
Moderate
Moderate OHSS, or grade 3 OHSS, characterized by presence of ascites in addition to the above symptoms.
Severe
Severe OHSS, which is further sub-divided into following grades:
- Grade 4, characterized by the above features and breathing difficulties.
- Grade 5, characterized by all the above symptoms in addition to change in the blood volume, increased blood thickness, abnormalities in blood clotting, and decreased kidney function.
Why does OHSS occur?
The release of an egg cell, ovulation, and maintenance of pregnancy thereafter should fertilization occur is regulated by the action of various hormones – luteinizing hormone (LH) and follicle-stimulating hormone (FSH) from the pituitary gland and estrogen and progesterone from the ovaries. Gonadotropin-releading hormone (GnRH) from the hypothalamus acts on the pituitary gland to release LH and FSH. These hormones stimulate the ovaries to release estrogen and progesterone. Should pregnancy occur, the presence of the fertilized egg leads to a rise in beta human chorionic gonadoptropin (HCG).
The entire process is regulated by feedback mechanisms. When certain hormones are too low, the stimulating hormone releases in larger quantities. When some hormones are too high, then the stimulating hormone is released in only small amounts. This is a simplified explanation for the monthly menstrual cycle and hormonal changes seen during pregnancy. However, in certain fertility treatments, the hormones are introduced into the body and continued beyond the ‘normal’ levels.
This leads to the signs and symptoms known as ovarian hyperstimulation syndrome. The hormone therapy causes cysts to form within the ovary and follicles to rupture. Certain substances then released by the ovaries cause the local blood vessels to become ‘leaky’ and more fluid leaves the blood vessels and enters the abdomen. Therefore fluid accumulation occurs within the abdomen and this is known as ascites. There may also be irritation of the inner lining of the abdomen (peritoneum) and this result in peritonitis.
Enlargement of the ovaries due to the presence of large cysts, coupled with distension of the abdomen have a host of effects like limiting movement of the diaphragm (difficulty breathing) and presses on the inferior vena cava leading to reduced cardiac output and low blood pressure. The fluid shift from the blood into the abdominal cavity leads to a decrease in blood volume. An electrolyte imbalance arises with this fluid shift which can then impact on kidney function. As the kidney becomes impaired, various other effects arises which further impacts on the blood composition and cardiac function.
Signs and Symptoms
Women who receive gonadotropin stimulation for inducing ovulation or undergo an assisted reproductive procedure (like IVF or in vitro fertilization) show signs and symptoms of moderate or severe ovarian hyperstimulation syndrome as early as a week after hCG (human chorionic gonadotropin) hormone treatment.
Late ovarian hyper-stimulation syndrome is usually severe and presents the symptoms about 2 weeks after taking hCG during implantation or pregnancy. The prresence of ascites, higher tendency of blood clotting, presence of fluid in body cavities, difficulty breathing, kidney failure, thickened blood, and abnormalities in electrolyte levels are common signs of OHSS.
Symptoms of OHSS may include the following:
- Breathlessness
- Abdominal discomfort
- Gastrointestinal symptoms (nausea, vomiting, diarrhea)
- Swelling
- Lethargy
- Sudden weight gain
Causes and Risks
The exact cause of ovarian hyperstimulation syndrome (OHSS) is not known; however the process is related to increase in permeability of blood vessels in the region around the ovaries. Ovarian hyper-stimulation syndrome affects women of childbearing age. The frequency of OHSS increases depending on the following factors:
- Extent of stimulation of ovaries, which will be accompanied with high levels of estradiol hormone and an increase in the number of ovarian follicles.
- Use of gonadotropins in combination with drugs called gonadotropin-releasing hormone (GnRH) agonists.
- Young age at conceiving.
- Low body weight and less body mass index (BMI).
- Presence of cysts (polycystic ovarian syndrome).
- Previous hyperstimulation treatment or history of OHSS.
- Increased number of small or medium follicles.
- High levels of estradiol around ovulation.
Tests and Diagnosis
The following tests are performed to diagnose ovarian hyper-stimulation syndrome (OHSS):
- Lab tests: Blood and/or urine samples are checked for hematocrit level (indicating percentage of red blood cells), blood clotting parameters, hCG and estradiol levels, liver and kidney functions, and to detect thickening of blood due to hemoconcentration.
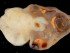
- Imaging tests like ultrasonography can detect the enlargement of the ovaries, presence of the follicles, and evaluate the ascites.
- Chest x-ray is performed in patients who complain of breathlessness.
The ultrasound video above shows both ovaries enlarged with cysts.
Treatment
Treatment of ovarian hyperstimulation syndrome is based on the symptoms presented. Ovarian hyperstimulation syndrome (OHSS) can be prevented or limited by carefully regulating levels of luteinizing hormone (LH) and hCG during ovulation.
Medication
Anticoagulants (like heparin, lepirudin, desirudin or enoxaparin) are given to OHSS patients to prevent blood clot formation. Electrolyte supplements are given intravenously to replenish blood volume. In some patients, blood components may also be given to increase plasma volume.
Surgery
In a procedure called paracentesis, fluid from the ascites accumulated in the abdominal cavity is removed to decrease pressure on the diaphragm and inferior vena cava. A tube can be placed between the lung cavities to remove the fluid from the region. Early surgical intervention in cases of internal bleeding, a ruptured cyst, or rotated ovaries can reduce the complications. However, surgery is rarely needed.
Supportive measures
Since ovarian hyper-stimulation syndrome often presents electrolyte imbalance, maintaining adequate hydration is considered very important.
In rare cases of severe ovarian hyper-stimulation syndrome, bed rest and maintaining fluid balance is recommended along with the medical treatment. Fast intravenous administration of normal saline is done for treating hypovolemia.
Critical care
For critical cases of ovarian hyperstimulation syndrome presenting kidney failure, liver damage, difficulty breathing and multi-organ failure, patients are admitted to critical care units. The following procedures are performed on such patients:
- Extra oxygenation is given.
- Dopamine is given intravenously in case of kidney failure to increase blood pressure.
- Anticoagulants are given to the patients.
- Pleural tap (thoracocentesis) is performed to remove fluid from the pleural space.
Complications and Prognosis
Untreated ovarian hyper-stimulation syndrome may cause multiorgan dysfunction and, potentially, death.The prognosis in patients presenting mild or moderate symptoms of ovarian hyperstimulation syndrome (OHSS) is excellent. However, the severe and critical cases of OHSS may result in death, if not treated promptly and adequately. Deaths from ovarian hyper-stimulation syndrome usually occur due to shock, electrolyte imbalance, internal bleeding, and the risk of a blood clot blocking a vessel.
References :
www.ncbi.nlm.nih.gov/pmc/articles/PMC3205536/
www.mayoclinic.com/health/ovarian-hyperstimulation-syndrome-ohss/DS01097