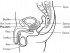
Prostate Cancer Treatments, Chemotherapy, Surgery, Radiation, Hormone
Prostate cancer patients with limited disease are grouped into low-risk, intermediate-risk and high risk for metastatic disease based on the clinical stage, Gleason score and PSA values. The treatment plan in limited disease is based on the risk.
- Low-risk group includes stage T1 or T2, Gleason score less than 7 and PSA values less than 10 ng/mL.
- Intermediate risk group is usually in stage T2, Gleason score of 7 and PSA value between 10 to 20 ng/mL.
- High risk group includes stage T3, has a Gleason score greater than 7 and PSA greater than 20 ng/mL.
The therapeutic options available for men with limited prostate cancer include :
- watchful waiting (wait-and-watch)
- androgen deprivation therapy
- radical prostatectomy with or without adjuvant radiotherapy of the pelvis
- radiation therapy (external beam radiotherapy or brachytherapy)
Early Stage Prostate Cancer
Low-risk to intermediate-risk prostate cancer
A watchful waiting (wait-and-watch / WAW) with delayed definitive therapy may be adopted with localized prostate cancer. Active intervention is initiated when unfavorable disease status or progression is evident on the annual follow-up surveillance prostate biopsy.
Radical Prostatectomy for Prostate Cancer
Radical prostatectomy is a major surgery and is recommended only in patients with a life expectancy of 10 or more years. It is usually performed in men with T1 or T2 prostate cancer which is clinically localized and without any serious comorbidity. The aim of surgery is the entire removal of cancerous tissue with negative excision margins and minimal loss of blood and other surgery-related complications.
Open surgery involves a suprapubic incision while a laparoscopic approach is the minimally invasive alternative option. The procedure also involves the removal of surrounding connective tissue and pelvic lymph nodes from both sides.
Radical prostatectomy can also produce excellent results when performed laparoscopically by experienced surgeons. Sometimes it may be performed with robotic assistance. The average hospital stay following radical prostatectomy is less than 3 days for open radical prostatectomy and 1 or 2 days for laparoscopic radical prostatectomy.
Radiation Therapy for Prostate Cancer
Radiation therapy, or radiotherapy, in prostate cancer is administered either in the form of external-beam radiotherapy (EBRT) or brachytherapy. EBRT and brachytherapy can provide results comparable to radical prostatectomy for patients with clinically limited prostate cancer.
The sophisticated computer-aided intensity modulated three-dimensional conformal radiotherapy (3D-CRT) which is currently used for radiation therapy reduces the volume of irradiated normal tissue and helps in safely delivering a high radiation dose to the prostate. The radiation of the pelvic lymph nodes in selected high-risk patients has been found to improve the outcome. Long term outcomes are significantly improved with use of higher dose of hypofractionated regimens particularly in high-risk patients.
Brachytherapy
Brachytherapy involves placement of temporary or permanent radioactive needles directly into the prostate tissue. Iodine-125 and palladium-103 isotopes are commonly used for permanent brachytherapy. Brachytherapy needles may be placed under TRUS guidance or transperineal ultrasound guidance. Brachytherapy alone provides adequate radiation to treat low-risk tumors that are limited by the capsule of prostate.
In intermediate and some high-risk prostate cancers brachytherapy is sometimes combined with EBRT. Brachytherapy is not ideal for prostate glands larger than 60 cm3. These patients may be prescribed androgen deprivation therapy to reduce the tumor size to a degree that will allow for the use of brachytherapy. Brachytherapy is usually avoided in patients who are experiencing significant urinary obstructive symptoms as there is a high risk of developing prolonged morbidity following brachytherapy. Patients with contraindications for EBRT (like patients who have small bowel close to the prostate or those with inflammatory bowel disease) are ideal candidates for brachytherapy.
Androgen deprivation therapy (ADT)
Androgen deprivation therapy is of value in intermediate risk patients in combination with EDRT. Improvement in the local control and prolongation of progression-free survival can be obtained with 4 months of ADT following EDRT. ADT alone is being used more frequently for patients who would like to have some therapy, but are not suitable for or decline radical prostatectomy or radiotherapy.
High Risk Prostate Cancer
Combined EBRT with Brachytherapy
A combination of external-beam radiation therapy (EBRT) and brachytherapy is considered to be suitable treatment option for patients with higher-risk prostate cancer. A high-dose rate temporary brachytherapy is sometimes preferred in the combination therapies.
Androgen Deprivation Therapy (ADT) and Radiation Therapy
Pelvic radiation therapy can be safely combined with neoadjuvant and concurrent ADT providing better results and is recommended for patients with locally advanced prostate cancer. Neoadjuvant ADT for 3 to 4 months before radiotherapy reduces the size of prostate and also acts like a radiosensitizer, thereby improving the effectiveness of the EBRT. ADT can also be continued as a long term adjuvant therapy to improve overall survival. Read more on radiation therapy under Prostate Cancer Treatments.
Radical Prostatectomy with Adjuvant Radiotherapy
High-risk patients who underwent radical prostatectomy but have positive margins, seminal vesicle involvement or detectable PSA are given adjuvant radiotherapy. This approach has shown to improve PSA progression-free survival and reduces the risk of a local recurrence.
Neoadjuvant ADT with Radical Prostatectomy
Neoadjuvant ADT significantly reduces positive margin rates and lymph node invasion. The combined approach outcome is significantly better than surgery alone.
Cancer Recurrence
Almost half of the men treated surgically or with radiation therapy show signs of recurrence and the most important sign being the rise in PSA levels. If the PSA is detectable after primary therapy, it either suggests the presence of cancer cells locally or at a metastatic site. Patients with a rise in PSA levels within 5 years following primary treatment are more likelyto experience a recurrence of the cancer. The chances of recurrence also depend on the clinical stage, Gleason score, and serum PSA level before the surgery.
Patients with signs of recurrence following radical prostatectomy may be treated with salvage radiotherapy which is potentially curative. Patients who fail to respond to radiation therapy may be considered for salvage radical prostatectomy. Other options for the patients include salvage cryotherapy, or brachytherapy. This can help in local control of disease and improve PSA progression-free survival. Patients who cannot be considered for definitive salvage therapies can be considered for ADT or surveillance (wait-and-watch approach). Treatment with ADT prolongs the time for progression in patients with PSA recurrence. The median time to development of metastases is about 12 years after the starting of ADT.
Advanced or Metastatic Prostate Cancer
ADT is the mainstay of treatment in the newly diagnosed metastatic prostate cancer patients. It can result in symptomatic improvement and disease regression in the majority of patients. The method adopted to produce androgen deprivation can vary between various centers. It can be achieved by surgical removal of testes (orchiectomy), medically with luteinizing hormone releasing hormone LHRH agonists, or use of anti-androgens.
LHRH agonists can temporarily increase testosterone levels in early days of therapy and cause an initial worsening of signs and symptoms. Usually an anti-androgen is also given in the first few days of LHRH therapy to prevent tumor exacerbation. The LHRH treatment can produce medical castration within 4 weeks. Most patients prefer sustained release LHRH-based treatments over the surgical approach. The high-risk localized, lymph node positive or recurrent prostate cancers remain sensitive to hormones for 5 to 10 years. The duration for which metastatic cancers remain hormone sensitive is usually short and lasts for about 2 years.
In some patients anti-androgens, like flutamide, are used alone or in combination with a 5-alpha reductase inhibitor, like finasteride. A close monitoring of PSA levels (refer to Prostate Cancer Diagnosis) after commencing with hormone therapy identify the patients at high risk for hormone-refractory prostate cancer.
Hormone-Resistant Prostate Cancer
Hormone-resistant prostate cancer (HRPC) is also called castration-resistant prostate cancer (CRPC) or androgen-independent prostate cancer (AIPC). Most patients with HRPC develop metastases to the bone which are detected on scans. The bone lesions are mostly osteoblastic (bone forming) lesions rather than osteolytic lesions. Bone lesions can be found in more than 80% of the HRPC patients and lymph node spread is found in 20 to 40% of HRPC patients.
The earliest indication of resistance to ADT is rising levels of PSA despite testosterone being in the range of castration levels (50 ng/dL or less). The patients are followed up with serial PSA levels. PSA decline and alkaline phosphatase levels are commonly used to assess response to treatment.
Patients having disease progression despite being on LHRH agonists and with castration level testosteron should continue with LHRH agonist treatment and additional secondary hormonal manipulation or chemotherapy should be considered. Secondary hormonal manipulation includes withdrawal of anti-androgen treatment (if present), suppression of adrenocortical secretions, glucocorticoids, or estrogens. In patients with bone metastases, bisphosphonates or radioisotopes concentrating in bone lesions may be useful in decreasing the rates of bone related events.
Patients on treatment with anti-androgens who developing HRPC should be evaluated for anti-androgen withdrawal response. Withdrawal responses for drugs like diethylstilbestrol, estramustine, megesterol and so on can also be evaluated in addition to androgen receptor blockers. If withdrawal responses are to develop, it usually takes 3-4 weeks (6-8 weeks for bicalutamide) after discontinuation of the medication. If no satisfactory response, additional treatments measures can be undertaken.
- Glucocorticoids have been shown to improve symptoms are produce PSA responses in HRPC patients. Prednisone or dexamethasone is commonly used for this.
- Estrogens have known palliative effects in HRPC patients, but its extensive use is limited by the high risk for thromboembolism. Diethylstilbesterol or premarin is now used only for palliative purposes. Estramustine which has estrogenic actions is also useful in HRPC for the same reasons.
- Drugs that suppress the adrenal steroid synthesis like ketoconazole can also be used in HRPC patients. Ketoconazole is often combined with low doses of glucocorticoids as the drug also reduces glucocorticoid levels. Ketoconazole is known to cause several drug interactions and hence the drug is used with caution with other drugs known to be involved in drug interactions.
- Zoledronate is the only bisphosphonate that is approved by FDA for HRPC with bone metastases. The drug effectively reduces the fractures related to bone metastases.
- Chemotherapy for non-metastatic HRPC is controversial. Chemotherapy regimens useful in metastatic HRPC are estramustine-docetaxel, docetaxel-prednisone or mitoxantrone-prednisone. Docetaxel based treatment is the only treatment that has shown improvement in the overall survival. Docetaxel-prednisone is now considered standard care for HRPC. Mitoxantrone has significant palliative effects as a single agent or in combination.
Complications of Treatment
It is important to note that the complications below will not arise in every case. Treatment should be undertaken by a cancer specialist (oncologist) in conjunction with other specialist physicians and the patient’s family doctor. The possible complications and other side effects should not detract from the need for treatment. In advanced cases, the various treatment modalities may be used for palliative care (comfort care) to improve the quality of life but not for “curing” the cancer. Refusing treatment advised by an oncologist due to the potential side effects and complications can ultimately delay appropriate treatment and reduce the chances of total cure.
Radical Prostatectomy
- Blood loss
- Injury to surrounding structures like rectum
- Deep vein thrombosis (DVT)
- Pulmonary embolism
- Bladder neck stricture
- Post-operative urinary incontinence
- Erectile dysfunction (ED)
Radiation Therapy
The radiation-related complications depend on the dose of radiation, the amount of normal tissue exposed to radiation and the field of irradiation. Acute complications of external radiotherapy usually start in the third or fourth week of treatment and often resolve with in a few days after the completion of radiotherapy.
- Radiation proctitis (inflamed rectum) – mucus discharge, rectal bleeding
- Fecal incontinence (mild)
- Chronic urethritis
- Urethral strictures
- Urinary incontinence
- Acute urinary retention
- Hemorrhagic/radiation cystitis
- Erectile dysfunction and other sexual function disruptions like decreased libido, absent ejaculate and decreased intensity of orgasm
Cryotherapy
The long term adverse effects with the current techniques of cryotherapy used for salvage therapy of prostate are :
- Erectile dysfunction
- Pain in rectum
- Urinary incontinence
- Urinary retention
- Urethritis
Androgen Deprivation Therapy
- Hot flashes
- Loss of libido
- Reduction in penile length and/or testicular size
- Erectile dysfunction
- Loss of facial and body hair
- Gynecomastia
- Breast tenderness
- Weight gain
- Muscle weakness
- Anemia
- Osteoporosis
- Hyperlipidemia
- Hyperglycemia
- Fatigue
- Depression
- Risk of cardiovascular disease and sudden cardiac events with ADT
Various preventive measures or therapeutic interventions are employed to minimize the adverse effects of ADT. Hot flashes are controlled with estrogens. Breast irradiation may be done prophylactically to prevent breast tenderness or gynecomastia. Osteoporosis can be prevented or treated with bisphosphonates. Cardiac risk factors are screened and treated according to the problems observed in each individual.
Chemotherapy
- Nausea
- Vomiting
- Abnormal taste sensations
- Fatigue
- Hair loss
- Loss of appetite
- Neuropathy
- Neutropenia