Gastroenteritis (Acute, Chronic) Causes, Diet, Foods to Eat, Avoid
What is gastroenteritis?
Gastroenteritis is the inflammation of the stomach, small and large intestine. The most common cause of gastroenteritis is due to the action of microbes or toxins, which irritate the lining in these areas of the gastrointestinal tract (gut) and affect nutrient absorption, trigger the process of inflammation and may lead to ulceration of the lining. A rare case of gastroenteritis known as eosinophilic gastroenteritis is associated with allergies and also cause inflammation of the stomach and small intestine. This results in the typical symptoms of nausea, vomiting, diarrhea and abdominal pain.
Acute Gastroenteritis
Infectious
Most cases of gastroenteritis are due to infections which are often acute in nature and will resolve spontaneously without treatment. Infectious gastroenteritis is known by many other common names like the stomach bug or gastric flu and is a result of an infection with a bacteria, viruses or protozoa. The incubation period may vary from a few hours in bacterial infections to a few days in viral gastroenteritis, while protozoal infections can take weeks before the onset of symptoms.
Read more on viral gastroenteritis.
At times, medical intervention may be necessary but this should only be considered when the causative organism has been identified and if the infection is not resolving. The symptoms of acute gastroenteritis are very intense with extreme nausea, violent vomiting and explosive diarrhea accompanied by severe abdominal pain being a typical presentation of infectious gastroenteritis. A fever is usually present.
Non-Infectious
Non-infectious causes like bacterial toxins, certain drugs (including chemotherapy), radiation therapy, poisoning and environmental toxins may also cause acute gastroenteritis. These cases of gastroenteritis may resolve once the causative factor is removed or expelled from the gut.
Chronic Gastroenteritis
Less frequently, a case of infectious gastroenteritis can be persistent – chronic in nature. A chronic case of infectious gastroenteritis is more likely to occur in an immunocompromised patient as is the case in HIV/AIDS (opportunistic infections) or a poorly managed chronic condition like diabetes.
A malabsorption syndrome is often a result of chronic gastroenteritis, irrespective of the cause, and leads to mineral and vitamin deficiencies.
Allergic
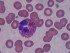
Eosinophilic gastroenteritis is another cause of chronic gastroenteritis but this condition is rare. It is closely related to other immune mediated conditions like hay fever, asthma and eczema (the allergic triad), especially in children. Food allergies are common in these conditions. Eosinophilic gastroenteritis is an inflammatory condition that affects the stomach and often the small intestine as well. A high concentration of eosinophils, a type of white blood cell, is found in the mucosal lining of the stomach and small intestine and these leukocytes play an important role in allergies.
Foods that Cause Gastroenteritis
Food infection is a term commonly used to describe food borne illnesses, where the microbe infects the host rather than by causing disease through toxins in the food (food poisoning or food intoxication). The most common foodborne illness is gastroenteritis but other diseases like Creutzfeldt-Jakob disease (CJD or “Mad Cow”disease) are also foodborne illnesses.
Although the term foodborne may indicate that it is only present in foods, waterborne illnesses may also be contracted in foods because contaminated water may be used for washing meat, fruits and vegetables that are eaten raw. Traveler’s should be aware of these foodborne diseases as it is a common cause of traveler’s diarrhea.
Food Sources
- Shigella spp may be present in any food.
Canned Goods
- Clostridium botulinum
Cheese (Unpasteurized)
- Campylobacter spp
- Enterotoxicogenic E.coli (ETEC)
- Listeria monocytogenes
- Salmonella spp
- Yersinia enterocolitica
Eggs (Raw)
- Salmonella spp
Meat (Beef, Pork) and Poultry (Chicken, Duck)
- Campylobacter spp
- Clostridium perfringens
- Enterohemorrhagic E.coli (EHEC)
- Listeria monocytogenes – hot dogs, vienna sausages, pate
- Salmonella spp
- Staphylococcus spp
Milk (Unpasteurized) or Juice
- Campylobacter spp
- Enterohemorrhagic E.coli (EHEC)
- Salmonella spp
- Staphylococcus spp
- Yersinia enterocolitica
Rice
- Bacillus spp
Seafood (Raw)
- Aeromonas spp
- Astrovirus
- Norovirus
- Plesiomonas spp
- Vibrio spp
Vegetables
- Aeromonas spp
- Clostridium perfringens
Bacterial Gastroenteritis
Bacterial gastroenteritis is the inflammation of the stomach and intestines (small and large) a result of a bacterial infection or the ingestion of bacterial toxins present in food. It is the cause of most cases of food poisoning or food infection and is prevalent where proper food storage and preparation methods as well as the availability of clean drinking water is lacking. Consuming partially cooked or raw meat as well as raw vegetables may also result in bacterial gastroenteritis. It is frequently seen in traveler’s diarrhea and gastroenteritis after eating at a restaurant or takeout foods.
What Happens in Bacterial Gastroenteritis?
A host of different bacterial species may cause gastroenteritis (Refer to the Stomach Bug Causes) and will act on the gut in a number of ways :
- Some bacteria will enter the gastrointestinal tract and attach to the lining (intestinal mucosa) where it will begin to secrete toxins (enterotoxins). These bacteria do not invade the cells of the intestinal mucosa. The toxins will affect nutrient absorption (malabsorption) and cause the mucosal cells to secrete electrolytes and water (secretory diarrhea). This will be evident as profuse, watery diarrhea with vomiting that usually starts in 12 to 48 hours after ingestion.
- Other bacteria may invade the mucosal cells leading to ulceration and bleeding. This causes inflammatory diarrhea which is associated with diarrhea that is sometimes bloody and there is significant abdominal pain.
- Bacterial toxins that are present in foods (exotoxins) tends to result in secretory diarrhea which is profuse and watery with nausea and vomiting that is very prominent. It is fast acting and symptoms may be evident in less than 12 hours after ingesting contaminated food. In some cases, the symptoms may be present in 1 to 6 hours.
This gastrointestinal irritation and inflammation causes the typical signs and symptoms seen in bacterial gastroenteritis – nausea, vomiting, diarrhea, abdominal pain with fever (not always present).
Treatment of Bacterial Gastroenteritis
- Antibiotics are not necessary in every case of bacterial gastroenteritis. Most cases are self-limiting and will resolve in a few days. If the causative organism has been identified with a stool culture and the symptoms are persisting, then antibiotics may be necessary. Immunocompromised patients may also require antibiotics.
- Antidiarrheal agents should be avoided unless the symptoms are persisting despite resolution of the infection or if antibiotics have already been commenced. This is dependent on individual cases and should be discussed with a medical doctor before using an antidiarrheal agent. A persistent diarrhea in this case may also require probiotics.
- Probiotics containing Saccharomyces boulardii and Lactobacillus casei may be useful in all cases but more so in the event of persistent diarrhea after the infection has been treated or has resolved.
- Oral rehydration therapy is the cornerstone of infectious gastroenteritis management. The BRAT diet followed by a simple bland diet should be commenced immediately once the vomiting subsides but an oral rehydration solution (ORS) should be continued for as long as the diarrhea is present.
Gastroenteritis Diet
Most cases of gastroenteritis (gastric flu, stomach flu, tummy bug) is due to infectious causes – viral, bacterial or protozoal. It is often self limiting and will resolve spontaneously with no need for treatment although proper oral rehydration is essential for the duration of the infection. The focus on gastroenteritis should be on management and the appropriate nutrition during this period is therefore essential.
Foods to Eat During Gastroenteritis
Eating solid foods is not practical due to the severe nausea and vomiting. Ideally the stomach should be ’empty’ as the regurgitation of food can result in aspiration into the lungs thereby leading to respiratory complications. However, the lack of sufficient nutrition can impair the body’s ability to overcome the infection. If the nausea is not severe, the BRAT diet may be commenced.
An oral rehydration solutions (ORS) should be started immediately. Soda and sports drinks are not suitable and a suitable ORS can be purchased from a drug store. This will prevent dehydration by replenishing fluid loss due to vomiting, diarrhea and sweating while limiting the irritation to the already inflamed stomach and intestinal lining.
- Oral Rehydration Therapy
- Types of oral rehydration solutions
- Quantity of oral rehydration solutions
Foods to Eat After Nausea and Vomiting
The focus should be on restoring a normal but bland diet as soon as possible. The foods that comprise the BRAT diet are usually better tolerated after a bout of nausea and vomiting.
- BRAT Diet
- Bananas, mashed
- Rice, soft
- Applesauce. grated apples, mashed boiled apples
- Toast, plain
Tea (black, decaffeinated) and yogurt may also be considered, however, it should be discontinued if it appears to aggravate the diarrhea.
Foods to Eat After the BRAT Diet
If the BRAT diet is well tolerated with no episodes of vomiting following consumption, a bland diet should be commenced as possible. This should include meat and vegetables as the body requires a good source of protein, fat and fiber to replenish its stores and nourish the system to help overcome the infection. It is advisable to use low-fat methods of cooking at the outset. Diarrhea may persist for a short period and an oral rehydration solution should therefore be continued.
Foods to Avoid During and Immediately After Gastroenteritis
Certain foods may irritate the gastrointestinal lining and could result in loose stool or prolong the diarrhea. These foods should be avoided and introduced in small quantities once the vomiting and diarrhea eases and the abdominal pain subsides.
- Fruits – citrus (orange, lemon, grapefruit)
- Hard legumes and grains – corn
- Drinks – caffeinated drinks (tea, coffee, cola) and alcohol
- Dairy
- Oily foods
- Spicy foods
Other foods that could trigger or aggravate diarrhea are mentioned in Inappropriate Diet and Diarrhea.
Last updated on August 15, 2018.