Hypothyroidism (Underactive Thyroid) Causes, Symptoms, Tests
The thyroid gland is the main regulator if the body’s metabolism. By the action of its thyroid hormones, thyroxine (T4) and triiodothyronine), the thyroid gland is able to stimulate metabolic activity, prompting the cells to take up more glucose from the bloodstream and break it down to yield energy. In the process, proteins are synthesized and lipids (fats) from the blood and adipose tissue (fat tissue) are used up.
The activity of the thyroid gland is regulated by the pituitary gland. Thyroid-stimulating hormone (TSH) from the anterior pituitary is secreted in response to thyrotropin-releasing hormone (TRH) from the hypothalamus. This mechanism keeps the thyroid activity in check and allows for a rise in metabolic rate during activity and a drop during low energy states like sleep.
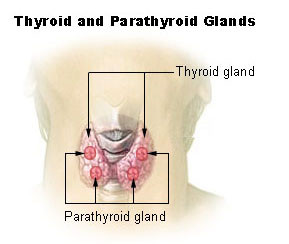
A ‘slow thyroid‘ is a common term for an underactive thyroid gland or hypothyroidism. It may involve diseases affecting the thyroid gland itself, or those that compromise the regulating mechanism in the anterior pituitary and/or hypothalamus.
What is hypothyroidism?
Hypothyroidism is the hypofunctioning (‘under-functioning’) of the thyroid gland leading to a deficiency of thyroid hormones, thyroxine (T4) and triiodothyronine (T3). Hypothyroidism can be labeled primary when the disease process is isolated to the thyroid gland or secondary when it involves the pituitary and/or hypothalamus with an otherwise normal thyroid gland. Most cases are primary hypothyroidism and often is a result of autoimmune diseases.
Hypothyroidism may be associated with enlargement of the thyroid gland (goiter) although this is not present in every case. When hypothyroidism is seen in infants or in early childhood, it is termed cretinism. It may also be seen with maternal hypothyroidism. Myxedema refers to hypothyroidism seen in the older child or adult. Overall hypothyroidism is seen more frequently in females than males.
Causes of Hypothyroidism
Most cases of hypothyroidism are primary meaning that the pathology involves the thyroid gland. Simply primary hypothyroidism can be classified as autoimmune, acquired and congenital. Some cases of hypothyroidism is due to unknown causes (idiopathic).
Autoimmune
This is the most common cause of hypothyroidism. Antibodies either causer inflammation of the thyroid gland (thyroiditis) or block the TSH receptors on the thyroid gland.
- Hashimoto’s thyroiditis
- Atrophic hypothyroidism
- Post partum thyroiditis
- Subacute (de Quervain’s) thyroiditis
- Grave’s disease with TSH-receptor blocking antibodies
Hashimoto’s thyroiditis is by far the most common cause in developed countries.
Acquired
Acquired causes may occur at any time in life and these days it is more often due to iatrogenic factors – hypothyroidism causes by medical treatment or diagnostic investigation. Some cases, like with viral infections, there is initially hyperthyroidism (overactive thyroid gland) followed by hypothyroidism (underactivity).
- Drugs used to treat hyperthyroidism (carbimazole), depression (lithium), arrhythmia (amiodarone), antibiotics (p-aminosalicylic acid)
- Thyroidectomy (surgical removal of the thyroid gland)
- Radioactive iodine
- Iodine deficiency
- Subacute (de Quervain’s) thyroiditis – possibly viral infection
Congenital
These are causes present from birth often due to inherited diseases.This may be seen as hypothyroidism in infants or only becoming evident later on in early childhood.
- Endemic iodine deficiency
- Dyshormonogenesis is a genetic defect that disturbs the multi-step process for thyroid hormone production.
- Thyroid aplasia – failure of the thyroid gland to develop or grow.
Secondary
Secondary causes is almost always due to a deficiency of thyroid-stimulating hormone (TSH) as a result of hypopituitarism (underactive pituitary gland).
Signs and Symptoms
The most characteristic signs and symptoms of hypothyroidism include :
- Fatigue. Severe tiredness and lethargy, after a little activity or for no apparent reason. This may also be experienced or interpreted as excessive sleepiness, diminished concentration, low energy levels or general ‘weakness’.
- Weight gain. The degree of weight gain may differ among individuals but it is usually a modest weight gain. This means that a person with a normal or healthy BMI (body mass index) will not gain weight to the degree that they will shift into the ‘obese’ category. Rather they may shift to the upper range of a healthy BMI or even fall into the overweight category.
- Sensitivity to cold. There is a noticeable intolerance to cold but should be differentiated from normal sensitivity to low temperatures. When related to hypothyroidism, the sensitivity to cold usually refers to an intolerance of low temperatures which were previously not a cause of discomfort.
In most cases, the presence or persistence of even one of these symptoms may warrant diagnostic investigation for low thyroid levels.
Other signs and symptoms, which may also be present, should not be immediately attributed to hypothyroidism, unless other possible causes have been excluded or if the one or more of the above symptoms are also present. These signs and symptoms may include :
- Depression
- Constipation
- Dry skin and/or dry, coarse (rough) hair.
- Weak or brittle hair and nails.
- Goiter – enlargement of the thyroid gland which is more common in Hashimoto’s thyroiditis.
- Menstrual changes – particularly menorrhagia, which is prolonged and/or heavy periods.
- High blood cholesterol levels.
- Intellectual impairment, such as difficulty concentrating, forgetfulness or poor memory, difficulty in completing certain mental tasks or may even present as personality changes.
- Pale skin
- Muscle aches
- Joint pains
- Leg swelling
- Puffy face
- Droopy eyelids
- Puffiness or swelling around the eyes
- Dull facial expression
- Hoarse voice
- Slow speech
- Macroglossia – enlargement of the tongue.
- Hypothermia – low body temperature.
- Anemia
- Vitamin B12 deficiency
- Carotenemia – orange discoloration of the skin.
- Bradycardia – heart rate under 60 beats per minute.
- Abnormal reflexes
- Psychosis known as ‘myxedema madness’.
- Pleural effusion – fluid or ‘water’ around the lung.
- Abdominal effusion – fluid or ‘water’ in the abdominal cavity.
- Numbness or tingling of the hands and feet (paresthesia).
Infants and Young Children
The thyroid hormones also regulate growth and therefore development will be retarded to some degree in congenital hypothyroidism or prolonged hypothyroidism in young children. The clinical features of cretinism include :
- Short stature
- Mental retardation
- Coarse facial features
- Protruding tongue
Older Children and Adults
These clinical features are seen with prolonged hypothyroidism and develop gradually over years. Older children may also have some features of cretinism.
- Physically and mentally slow
- Poor memory
- Hoarse voice
- Shortness of breath
- Enlargement of the tongue
- Non-pitting edema (pretibial myxedema)
Myxedema Coma
Myxedema is the medical term for severe hypothyroidism resulting in number of serious symptoms caused by the severity of the low thyroid hormone levels as well as the prolonged state of hypothyroidism. This state usually occurs in case of undetected, misdiagnosed or a poorly managed case of hypothyroidism.
Myxedema coma is a life-threatening complication of severe hypothyroidism and is triggered by exposure to cold, trauma, infection or drugs that suppress the central nervous system (like ‘sleeping tablets’, anesthetics or in alcohol abuse). Characteristic features of myxedema coma is a coma with hypothermia (low body temperature), depressed or absent reflexes (areflexia), shallow breathing, hypoxia, seizures and reduced blood flow to the brain. Immediate medical treatment is required or death may occur.
Underactive Thyroid Blood Test Levels
Your doctor may request any or all of the following :
- Total or Free T3 level
- Total or Free T4 level
- TSH level
- Thyroid antibodies
Most thyroid hormones, T3 and T4, in the blood is bound to proteins. However a small proportion of these hormones remain unattached to any protein and this is referred to as the free T3 or free T4 level.
Thyroid antibodies are formed in autoimmune diseases, like Hashimoto’s thyroiditis, and the antibodies trigger the body’s immune cells to ‘attack’ the thyroid gland, which causes inflammation and hampers the production and secretion of the thyroid hormones. The thyroid antibody test is not routinely conducted but may be requested based on your doctor’s discretion after the initial thyroid profile results.
It is not advisable to diagnose your thyroid condition based on actual values but rather use it as a guide for future medical consultations with a doctor. Values may fluctuate due to a number of reasons, and age, past medical history and current drug schedule should be taken into consideration before any diagnosis is made. All blood test reports are presented with a reference range, which indicates the normal value range for a specific test. Using the reference range as a guide, you will be able to identify values that are low, normal or high.
Ensure that any reference range that you may be using, which is not on the report, is based on the same measurements as your report. Due to the difference is measurements among different countries, type of test requested, methods or individual labs, as well as the variation in readings due to individual factors, may determine differences between low, normal or high values in each case.
Normal
Low
Low
Normal
Low
Low
High
High
Low/Normal
Mild Hypothyroidism
Hypothyroidism
Secondary Hypothyroidism
Secondary hypothyroidism is a result of low secretion of TSH from the pituitary or the low secretion of thyrotropin-releasing hormone (TRH) from the hypothalamus. A thyrotropin-releasing hormone (TRH) test may have to be done to confirm a reduced TRH secretion.
Under certain circumstances, your doctor may diagnose a condition known as euthyroid sick syndrome (ESS), where the thyroid gland and regulating mechanism is normal but there are low levels of thyroid hormones (T3 and T4). These low levels may be due to other conditions that are not related to the thyroid gland but the symptoms of low thyroid are usually present.
In euthyroid sick syndrome, blood tests will reveal a low T3 and T4 level but a normal TSH level. Even if the TSH level is moderately high or low in euthyroid sick syndrome, it will not be affected to the level recorded in hypothyroidism. Possible causes of euthyroid sick syndrome include fasting or starvation, calorie restriction diets, eating disorders, low protein intake, renal failure, myocardial infarction (heart attack), cirrhosis, diabetic ketoacidosis, sepsis and trauma.
References
- Hypothyroidism (Myxedema). Merck
- Euthyroid Sick Syndrome. Medscape
- Thyroid Panel. Lab Tests Online
Last updated on August 31, 2018.