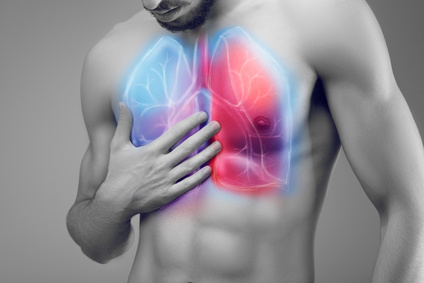
Pus In and Around the Lung (Abscess vs Empyema)
Pus is a fluid that forms in and around infected tissue. It consists of dead immune cells, tissue particles and bacteria. Sometimes this pus may be walled off in an isolated area. We refer to this as an abscess. At other times the pus may exist in cavities and around organs. This is known as an empyema. Both an abscess and empyema can occur in and around the lungs.
What is a lung abscess?
A lung abscess is a collection of pus in the lung. It occurs with an infection and tissue destruction. It is also known as a pulmonary abscess.. A lung abscess is the consequence of infectious microorganisms, particularly bacteria, entering or invading the lung tissue. It may occur either as a solitary abscess (single) or multiple abscesses.
Any pathogen can cause abscess formation but anaerobic bacteria are the most likely microorganisms to do so.
If the abscess develops in an otherwise healthy lung and respiratory tract, then it is considered as a primary abscess. It can also develop as a complication of some underlying lung pathology – secondary abscess. The size of a lung abscess can vary from a few millimeters in diameter to several centimeters (up to 5 to 6 cm). The abscess may connect with an air passage (usually the bronchus) and then partially drain and become filled with air. The pus may then be coughed up (sputum). The abscess could also connect with and drain into the pleural cavity which may then lead to an empyema (fluid around lungs – pus).
What causes a lung abscess?
The most common cause of a lung abscess is when microorganisms from the mouth pass through the respiratory tract to reach the lung tissue. This causes aspiration pneumonia and the death and destruction of the lung tissue (necrotizing pneumonia) progresses to abscess formation. It is more likely to occur if the patient has poor oral hygiene, several tooth cavities, gingivitis or periodontitis.
Aspiration occurs in a person who is intoxicated (alcohol, narcotic drugs) or sedated (anesthesia, opioid painkillers). Those with neurological disorders, particularly the elderly, and other causes of swallowing difficulties (dysphagia) are more prone to aspiration pneumonia. Saliva, food or inhaled foreign objects may carry these pathogenic microorganisms into the respiratory system. Most cases are due to anaerobic bacteria although mixed bacteria (anaerobic and aerobic) account for almost half of all cases. Other pathogens include fungi, mycobacteria and parasites.
A lung abscess may also be caused by an infection spreading from a neighboring site (direct infiltration), like with a liver abscess, subphrenic abscess or pleural infection (infectious pleuritis), or from distant sites via the blood stream (hematogenous spread) like with bacteremia or septic embolus associated with tricuspid endocarditis. It may also develop as a secondary infection in pre-existing respiratory disease like bronchiectasis or bronchial/lung cancer.
Signs and Symptoms of a Lung Abscess
Most of the signs and symptoms are non-specific and may be seen in most other infectious diseases of the respiratory tract and lungs. This includes:
- Productive cough
- Breathlessness
- Pleuritic chest pain
- Fever often with rigors
- Profuse perspiration
However, the expectoration of copious amounts of foul smelling sputum, which is often blood-stained, should raise the concern about a lung abscess. Patients will also report that the sputum is foul tasting leaving a persistent bad taste in the mouth. Digital clubbing is seen after several weeks.
Rapid breathing (tachypnea), rapid heart rate (tachycardia) and abnormal breathing sounds (crackles / bronchial breathing) associated with pulmonary consolidation and pleural effusions may also be seen. General symptoms include dehydration and weight loss.
What is an empyema?
An empyema is when pus collects in a body cavity. It is most often used to refer to pus in the pleural space, which is the space around the lungs. The more accurate term is a pleural empyema. Other areas of pus collection are usually designated as such, for example empyema of the sinus, referring to collection of pus within the paranasal sinus. Interstitial fluid, blood and even lymph can also collect in the pleural space. Read more on fluid around the lungs.
Pus is a combination of inflammatory infiltrate with lymphocytes, cellular debris and microbes. Varying amounts of blood, often degraded, is also present. It may originate from an infection of the pleura (pleuritis), often secondary to a lung infection (pneumonia). Seeding of the pathogen, usually bacteria but sometimes fungi, within the pleural space leads to pus formation and accumulation. Pus may also drain from a neighboring site into the pleural space, as is seen with a ruptured lung abscess and the development of bronchopleural fistula.
Causes of an Empyema
Most cases of an empyema are related to bacterial pneumonia (infection of the lung). Pneumonia tends to cause a pleural effusion – para-pneumonic effusion. This can be uncomplicated (containing exudate), complicated (exudate with high concentrations of neurophils) or empyema thoracis (pus in the pleural space). An empyema associated with bacterial pneumonia, or other lung infections including tuberculosis (TB), is a complication. Early treatment and proper management of pneumonia would reduce the chances of an empyema.
Other causes of an empyema may include spread from a ruptured subphrenic abscess, cardiothoracic surgery, sharp force trauma to the chest, esophageal rupture and following drainage of a pleural effusion (thoracentesis). It may also occur as the infection spreads from the neighboring cavities – peritonitis or mediastinitis.
Signs and Symptoms
An empyema is usually one-sided (unilateral). The pus may fill the entire pleural space or only part of it (loculated). The symptoms of an empyema are not always obvious as it tends to occur in the backdrop of a lung infection. It should be suspected if the symptoms of an infection does not resolve despite treating the primary infection with the suitable antibiotics.
Recurrence of a lung infection may also be an indication of undetected empyema. Symptoms of an empyema are similar to that of a pleural effusion and includes :
- Pleuritic chest pain – worse when breathing in or coughing
- Dry cough
- Excessive perspiration, night sweats
- Fever with rigors
- Difficulty breathing – may be absent, mild, moderate or severe
- Weight loss
- Malaise