Prostate Biopsy Procedure, Preparation, Anesthesia
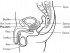
Prostate biopsy is a procedure in which small tissue samples are taken from the prostate gland and is examined under a microscope for the presence of cancer.
When is the biopsy done?
A prostate biopsy is highly recommended in patients if the digital rectal examination (DRE) is abnormal, irrespective of PSA (prostate specific antigen) status. Even if the findings upon a digital rectal examination are normal, an elevated PSA levels may also prompt the need for a biopsy.
PSA Guidelines for a Biopsy
A prostate biopsy is normally recommended when the PSA (Prostate Specific Antigen) blood test values are > 4 ng/mL.If the values are between 2.6 – 4 ng/mL, then a prostate biopsy is optional.
If the rate of change of PSA values (PSA velocity) over a period of at least 18 months (a minimum of three values needed to calculate PSA velocity) is found to be > 0.35 ng/mL/year, then a prostate biopsy is recommended.
If a patient with normal DRE and PSA between 4 – 10 ng/mL cannot be biopsied, then percent-free PSA levels can be used for management.
- If percent-free PSA levels are >25% then annual follow ups with DRE and percent-free PSA may be considered.
- If percent-free PSA levels are between 10-25%, a prostate biopsy is preferrable.
- If percent-free PSA levels are <10%, a prostate biopsy is highly recommended.
Other Factors to Consider
In men with two prior negative extended-pattern prostate biopsies, a saturation biopsy may be done in selected situations like :
- elevated PSA that is persistently rising,
- or histologic evidence of atypical cells (abnormal cells),
- or high grade intraepithelial neoplasia on prior prostate biopsy.
Types of Prostate Biopsy
Traditional prostate biopsies can be classified based on the approaches adopted in the procedure. There are 3 types namely :
- Transrectal – biopsy performed using a probe passed through anus into the rectum
- Transurethral – biopsy performed using a probe passed through the urethra)
- Transperineal – biopsy done through the skin in front of the anus
Saturation biopsy (prostate mapping) is a modified type of transperineal prostate biopsy that has higher degree of accuracy.
Preparation for a Biopsy
- A patient may be given antibiotics before the procedure to prevent any infection (especially for the transrectal procedure) following the biopsy.
- An enema will be done before the biopsy to empty the feces and gas from bowel, which may complicate the procedure.
- The patient is also required to discontinue drugs like aspirin, one week before the procedure to reduce the chances of bleeding.
- Patients who are biopsied under general anesthesia are required not to eat anything orally at least 6 hrs before the procedure and not to drink anything at least 4 hours prior to the procedure.
Anesthesia for Prostate Biopsy
Anesthesia reduces any discomfort during the procedure which is a common complaint among patients undergoing a prostate biopsy.
Local anesthesia is safe and effective. It can be done with topical lidocaine gel or periprostatic nerve block with injection of lidocaine or bupivacaine. The topical lidocaine is effective in reducing the discomfort during probe insertion while the periprostatic injection or nerve block is more effective in minimizing the pain during the biopsy itself.
General anesthesia is required in patients undergoing transperineal saturation biopsy. Intravenous sedation or general anesthesia may be required in certain transrectal or transurethral biopsy patients who are not adequately anesthetized with nerve block or if the patients are found to have anal or urethral strictures.
Prostate Biopsy Procedures
Transrectal Prostate Biopsy
A transrectal prostate biopsy is the technique recommended by the NCCN (National Comprehensive Cancer Network). The patient is placed in the left lateral position. The probe is inserted through the rectum into the anus and guided by a transrectal ultrasound (TRUS). Based on the necessary scheme planned for the patient for a correct diagnosis, 6 to 12 systematic samples are taken using a spring-loaded biopsy gun.
Palpable abnormalities on DRE (abnormal areas felt by the doctor during a digital rectal examination) may also be targeted for biopsy using finger guidance and abnormal areas visible on TRUS are also be sampled. Each core sample should be identified separately with the location and orientation noted. This is necessary for the histopathologist to report on the grade of cancer, if present. It also helps to identify the extent of malignancy.
A transrectal prostate biopsy is usually an outpatient procedure and is quick, effective and relatively painless.
Transurethral Prostate Biopsy
The transurethral biopsy is also an outpatient procedure, performed under local anesthesia, in which the biopsy is done through the urethra with the help of an illuminated cystoscope. This approach helps the doctor to see the area directly (direct visualization) when biopsying the prostate gland.
The doctor inserts a cutting loop through the cystoscope to extract the tissue sample for pathological examination. The cutting loop extracts a small amount of tissue with each turn. The samples are then sent for histopathology.
Transperineal Prostate Biopsy
Patients are placed in the lithotomy position – lying on the back with knees bent and legs elevated. The ultrasound probe (TRUS) is inserted into the rectum. An automated biopsy gun with spring-loaded needles are used to collect the samples based on the areas isolated through ultrasound. Samples are then sent to be analyzed by a histopathologist.
Saturation biopsy
This is also known as a transperineal template-guided saturation biopsy or prostate mapping. It requires hospitalization as general anesthesia is necessary although the procedure takes only about 30 to 45 minutes. Ideally an MRI scan is conducted prior to the biopsy.
A TRUS probe is passed through the rectum and a grid with holes every 5mm is placed on the skin that lies in front of the anus. A biopsy needle is inserted through each of the hole and sample of prostate is taken from every 5mm. A total of 30-50 biopsies are done and each biopsy sample is placed in a separate container for the histopathologist to examine.