Staph Skin Infections Pictures
Staph Skin Infection Pictures
Staph (pronounced staf) skin infection may appear as :
- a red bump or pus-filled blister (folliculitis)
- a boil (furuncle)
- infected cystic acne, hidradenitis suppurativa, pilonidal cyst
- a vesicle which may burst and crust over (impetigo)
- an erythema (cellulitis)
- a skin scalding (staphylococcal scalded skin syndrome)
- an infected wound or burn
Drainage of pus from lesions is common.
What Causes Staph Skin Infections?
Staph infections are mainly caused by bacterium Staphylococcus aureus, and rarely by S. epidermidis, or S. saprophyticus. In staph carriers, S. aureus lives in the nose and on the skin, less commonly in the mouth, mammary glands, urinary, intestinal and upper respiratory tract (1). Staphylococcal infections usually remain localized at the site of entry. What is Staphylococcus aureus?
Who Is at Risk for Staph Infections?
People at greatest risk of contracting a staph infection are :
- Staph carriers (many individuals who carry S. aureus in the nose, throat or skin; 20-30% of people are colonized persistently, especially health care workers, patients with diabetes and those on dialysis)
- Newborn infants
- Breastfeeding women
- Obese persons
- People living in crowded communities or hot climates
- Those with skin injuries or surgical wounds
- Persons with piercings and fresh tattoos
- Persons with skin diseases, like atopic dermatitis or seborrhea
- Persons with weak immune system, diabetes, cancer, vascular, blood or lung disease
- Patients receiving oral steroids or chemotherapy
Are Staph Skin Infections Contagious?
Staph skin infections are fairly contagious. It can spread by :
- Skin to skin contact with an infected person
- Sharing razors, towels, clothes, bed linens, sport equipment (athletes!), toys
- Walking barefoot or sitting around swimming pools
- Contact with infected pets
- Auto-infection by nose picking and skin scratching
- Sneezing – when droplets from the nose of infected person (or staph carrier) fall on an injured skin of another person.
Read more on staph epidemiology.
Folliculitis
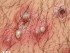
Staphylococcal folliculitis affects hair follicles on the face, scalp, neck, trunk or limbs but not the hands, soles and mucous membranes where there are no hair follicles. Folliculitis usually appears as a group of red bumps, which may develop into pus-filled blisters (Picture 1). Itch or pain are main symptoms; follicles may open and drain pus. Low grade fever may be present. Folliculitis barbae is a folliculitis of the beard in men. A stye or hordeolum is folliculitis affecting one or more hair follicles on the edge of the upper or lower eyelid.
Picture 1. Folliculitis
(source: Samuel Freire da Silva, M.D., Atlasdermatologico)
More Folliculitis Pictures.
Boil – Skin Abscess
A boil or skin abscess is a collection of pus in the skin from various causes. Boils may appear as red colored nodules which are tender, itchy or painful. A boil often opens at some point of growth and drains pus.
A furuncle develops from an infected hair follicle, when the adjacent skin tissue is involved. It most commonly appears on the neck (Picture 2), arms or legs as a red nodule up to 1 cm in size, and usually after some time opens and drains pus. Furuncles may be itchy and painful and low grade fever may be present. It usually heals on its own. When several furuncles coalesce, it forms a carbuncle. Carbuncles most often appear on the nape of the neck in persons with lowered immunity, friction of clothes or bad hygiene (9).
Picture 2. Furuncle on the neck
(source: Samuel Freire da Silva, M.D., Atlasdermatologico)
Cystic acne is a large collection lesions caused by oil and dead skin cells trapped in the sebaceous glands, mostly occurring on the face of teenagers.
Hidradenitis suppurativa are boils appearing in armpits, groin, anal area or under the breasts and inner thighs – areas which are often rubbed and are rich in the sweat and oil glands. The condition usually appears in puberty, it worsens with time and may persist for years. Sebaceous glands produce excessive oil due to increased hormonal activity. Sweat glands may be clogged due to excessive sweating and shed skin cells.
Hair follicles may then be infected by staphylococci. When all these disorders merge, it results in a group of tender red nodules, under-skin lumps filled with pus and black-heads. Hormone changes, stress, obesity and excessive sweating may aggravate symptoms. Antibiotics and isotretinoin may help in some cases, but surgical removal of nodules is often required (8).
A pilonidal cyst arises from irritated and infected hair follicles in the area between the buttocks, often due to prolonged sitting (during trips). Surgery is often required to remove the cyst completely.
Cellulitis – Deep Skin Infection
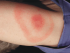
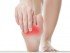
Cellulitis is an infection of the underlying skin tissue, appearing as a red, swollen, warm, tender skin patch of various size (Picture 3). An infection usually starts when Staphylococcus aureus (or group A streptococci, or rarely other bacteria) enter through the skin wound and spreads under the skin. The legs and arms are most commonly affected. Fever is usually present and the local lymph nodes may be swollen (2). Cellulitis always needs to be treated – oral antibiotics are usually prescribed.
Picture 3. Cellulitis on the shoulder (source: phil.cdc.gov)
A superficial skin infection called erysipelas is usually caused by streptococci or, rarely, by staphylococci (2).
Impetigo
Impetigo is a crust-forming staph infection of the skin, mainly occurring in pre-school children. In adults it may follow other skin disorders like atopic dermatitis. It is highly contagious and easily spreads to other parts of the skin. Fever is not common, but the local lymph nodes may be affected. Infection usually heals on its own in 2-3 weeks (3). It most often occurs in summer and autumn.
Impetigo contagiosa starts like red bumps which rupture, ooze fluid or pus, and form honey colored crusts. It mostly appears around the child’s nose and mouth (Picture 4).
Picture 4. Impetigo
(source: Samuel Freire da Silva, M.D., atlasdermatologico)
Bullous impetigo mostly appears in infants in the form of vesicles of various size on the trunk or limbs. Ecthyma is a severe form of impetigo with thick crusts. It affects deeper layers of the skin, it is painful, it may develop into an ulcer and leave scars.
Complications of impetigo are rare and include scars, permanent hypo- or hyper-pigmented skin patches and cellulitis.
Paronychia
Paronychia is an infection of the skin folds of the nails (Picture 5). Acute paronychia is usually caused by staphylococci, other bacteria or herpes virus; chronic paronychia is usually caused by fungi. It may follow nail biting, finger sucking, wearing artificial nails, ingrown toenail, or may appear in people who constantly have wet hands (like bartenders or dentists). It appears as a painful, red swelling around the nail or as red bumps or blisters.
The nail may change its color or become detached. Soaking an affected finger in warm water few times a day may help to relieve pain. Paronychia heals on its own; if not, a skin cut and pus drainage are needed. Sometimes a part of the nail has to be removed (4). Rarely, infection spreads toward the tendons and bones, or bacteria invade into the bloodstream.
Picture 5. Acute paronychia
Source: Wikipedia
Wound Staph Infection
Staph is the most common external cause of wound infections. In surgical wounds, bacteria E.coli and enterococci are often involved.
Symptoms and Signs of Wound Infection
A wound infection may develop from 48 hours to 30 days after an injury or surgery.
Mild wound infection symptoms and signs may include (5):
- Skin around the wound becomes increasingly red (cellulitis), swollen, warm and painful
- Pus or cloudy fluid is draining from the wound
- A crust may form on the wound edges, or an existing crust is increasing in size
Symptoms and signs of severe wound infection:
- A red streak (from inflamed lymphatic vessel) is spreading from the wound toward the local lymph nodes (usually in the armpits or groin), which may be swollen and tender.
- Body temperature over 100°F (37.8°C).
- Poor wound healing.
- Foul odor from the wound.
- A bluish or black gangrenous tissue around the wound.
Treatment of Infected Wounds
Open infected wounds should be cleaned with a suitable antimicrobial solution and preferably dressed by a medical professional. Oral antibiotics will usually be prescribed. With treatment, the symptoms should start to ease within 2 to 3 days, and completely resolve within 7 to 10 days. To relieve pain acetaminophen or ibuprofen can be used, if temperature especially if the temperature exceeds 102F° (39°C).
Treatment of Infected Burns
In mild burns topical antibacterial ointments, like mupirocin, can be used to prevent infection. In severe burns, systemic antibiotics and surgical treatment are needed.
Staphylococcal Scalded Skin Syndrome (SSSS)
Staphylococcal scalded skin syndrome (SSSS) is an extensive red rash, like scald, caused by toxins released by Staphylococcus aureus. It mostly appears in children under 5 years of age who do not have enough antibodies to fight staph toxins. Staphylococcal scalded skin syndrome in newborns is sometimes called pemphigus neonatorum. Connections between skin cells are cleaved by staph toxins, resulting in scalding.
A disease may start as a common staph skin infection, like impetigo, from which toxins are released. Fever, irritability and skin redness may follow in a couple of days, and then red blisters, paper-like skin wrinkling and scalding appear in one or more skin areas.
Diagnosis is by a skin biopsy. Treatment by intravenous and later by oral antibiotics usually results in complete healing in 5-7 days without consequences (7). The most dangerous complications are dehydration and sepsis. Staphylococcal scalded skin syndrome in adults with lowered immunity may be followed by life threatening pneumonia and sepsis.
Staphylococcal scalded skin syndrome is highly contagious and it often outbreaks as epidemic in kindergartens; in this case, children should stay at home.
Treatment of Staph Skin Infections
Mild staphylococcal folliculitis or furuncle may disappear in a few days or couple of weeks with good hygiene, showering and wearing fresh airy clothes.
In persistent skin infection, like carbuncles, oral antibiotics, like dicloxacillin or cephalosporin, are effective. If MRSA is diagnosed, clindamycin, trimethoprim-sulfamethoxazole, levofloxacin, minocycline or linezolid may be used (2). Boils with an opening (cap) may need to be incised and drained of pus. The area is appropriately dressed. The dressing has to be changed and underlying skin cleaned every day until the boil heals completely. A large abscess may require a surgical drainage.
In infected wounds, stitches or foreign bodies have to be removed. Any dead tissue (necrotic) has to be surgically removed.
Extensive skin infections, like in staphylococcal scalded skin syndrome (SSSS), require intravenous antibiotics. Antibiotics should be chosen on the basis of antibiotic susceptibility test.
Remedies in Staph Skin Infections
Topical antibacterial treatment. Fusidic acid (Fucidin®) and mupirocin (Bactroban®) are available as ointments. Triple-antibiotic (neomycin, polymyxin and bacitracin) mixtures can be found in pharmacies. Treatment should last up to 10 days, and administered 2 to 3 times a day. Longer use should be avoided to prevent bacterial resistance. Some ointments may cause dry skin, burning or rash.
To prevent spread of an infection to other skin areas, antibacterial soaps, bath additives, and creams containing chlorhexidine, triclosan and povidone-iodine can be used.
To reduce itch, especially in children, emollients may be used.
To treat nasal staph carriage, nasal mupirocin ointment or oral rifampin may be used (4,2). Nasal swabs should be taken from the patient and his/her family members to identify staph carriers.
Laser hair removal helps in recurrent folliculitis.
How to Prevent Staph Skin Infections?
People prone to get recurrent staph skin infections should:
- Regularly wash their hands, avoid nose picking, nails biting and skin scratching.
- Use electric razor instead of blades or shave less frequently.
- Wear fresh, comfortable, airy clothes.
- Clean athletic equipment and seats beside pools before using.
- Do not share razors, towels, clothes, bed lining with others.
- Treat any underlying diseases, like diabetes or dermatitis.
References:
- Staph carriers (merck.com)
- Cellulitis and erysipelas (skininfection.com)
- Impetigo (mayoclinic.com)
- Paronychia (nlm.nih.gov)
- Wound infection (med.umich.edu)
- Infection of surgical wounds (emedicine.com)
- SSSS (dermnetnz.org)
- Hydradenitis suppurativa (mayoclinic.com)
- Carbuncle (nlm.nih.gov)