Calcinosis Cutis (Calcium Deposits in the Skin)
Definition
Calcinosis cutis is a condition where there are deposits of calcium salts in the skin. It may also extend to the underlying tissue known as the subcutaneous tissue and calcinosis can occur even deeper in the body including within muscles or organs. In calcinosis cutis, the abnormal deposits are made up of calcium salts and not bone as is the case with osteoma cutis.
When abnormal calcium deposition occurs in the soft tissues within the body, it can cause functional disturbances some of which can even be fatal in the long term. However, the prognosis is not usually as serious with calcinosis cutis. The condition can lead to severe disfigurement, superficial pain and skin ulcers. In rare instances, it can lead to gangrene due to blockage of blood flow.
Incidence
Calcinosis cutis is not a common condition and the exact incidence is not known. It tends to affect both males and females equally. Depending on the type of calcinosis cutis, the condition may more commonly be seen in childhood, adolescence or early adulthood. Calcinosis cutis can affect any person of any ethnicity but is more common among Africans, particularly those of South African origin.
Pathophysiology
Calcium is a one of the major minerals in the human body. Most of the calcium is stored within the bones but trace amounts are utilized by every cell in the body. Normally the body keeps the calcium levels in the bloodstream and other body fluids within a narrow range. This prevents metabolic disturbances of calcium from arising. However, when the normal limits are exceeded, calcium deposition can occur in a number of different tissue including the skin. It works synergistically with phosphate, another abundant mineral in the human body. Therefore the deposits are primarily calcium phosphate salts and calcium carbonate is present to a lesser extent. Deposition occurs in the dermis of the skin but may extend to the underlying subcutaneous tissue.
The exact mechanism behind calcium deposition in the skin is not completely understood. It can occur in the backdrop of high calcium and phosphate levels in the blood and tissue fluid. This may lead to a high calcium level within the cells as well and precipitation of calcium is possible, in much the same way as calcium stones form in the kidney. Tissue damage may also be a trigger as certain exposed proteins then bind phosphate even if the calcium and phosphate levels are normal. Calcium subsequently binds with the phosphate leading to the formation of calcium deposits.
Types
There are four major types of calcium calcinosis classified according to the underlying cause :
- Dystrophic
- Metastatic
- Idiopathic
- Iatrogenic
Dystrophic Calcinosis Cutis
This type of calcinosis cutis arises in areas where the tissue is damaged. Any type of inflammation, malignancy or even tissue death appears to be the precipitating cause. Dystrophic calcinosis cutis is the most common type.
Metastatic Calcinosis Cutis
This type of calcinosis cutis arises when the levels of calcium and phosphate are abnormally high. Therefore any condition that cause hypercalcemia or hyperphosphatemia can lead to metastitis calcinosis cutis.
Idiopathic Calcinosis Cutis
Idiopathic is the medical term for a condition due to unknown cause. In this case, calcinosis cutis occurs for no clearly identifiable reason. The calcium and phosphate levels are normal and there is no preceding tissue damage. The patient is not using any drugs and has not undergone any medical procedures that are linked to calcinosis cutis.
Iatrogenic Calcinosis Cutis
This is a type of calcinosis cutis that arises as a consequence of using certain medication or undergoing certain medical procedures. It arises secondary to medical treatment and procedures and can sometimes resolve once the medication is discontinued.
Location
The location where the calcium deposits in the skin occurs can vary among individuals and even with certain causes. In the most common type, dystrophic calcinosis cutis, the deposits arise at the site of tissue damage. With metastatic calcinosis cutis, the deposits tend to occur around the large joints in the body such as the shoulders and knees. In iatrogenic calcinosis cutis, the deposits tend to occur at the site where the medication is administered or point of entry into the skin with certain medical procedures.
Symptoms
The calcium deposits in the skin tend to grow gradually and there are usually no symptoms present. There may be symptoms of the underlying disease or condition that precipitates the onset of calcinosis cutis may be evident.
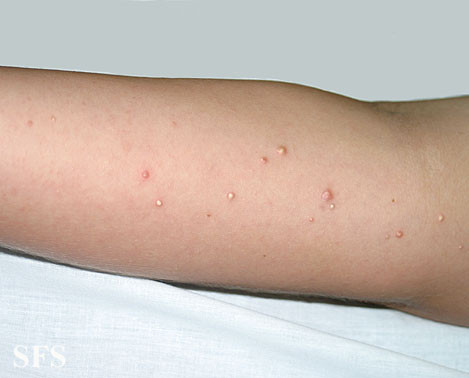
- Once grossly evident, the deposits appear as white to yellow pimples, patches or nodules.
- The lesion is firm as calcium tends to form a hard mass.
- Tenderness may develop and can sometimes be painful on the sensitive parts of the body like the fingertips.
- Ulceration of the lesions are usually tender and painful.
- Ulcers may ooze a chalk-like discharge which is cream in color.
- Large deposits near the joints can cause joint stiffness and mobility may be restricted.
- In very severe cases, the skin may become gangrenous at the affected site.
Pictures
Calcinosis cutis pictures from Dermatology Atlas Brazil courtesy of Samuel Freire da Silva, M.D.
Causes
The exact reason why calcinosis cutis occurs, even when precipitating conditions are known, is not always clear. Not every person who has these predisposing factors will develop calcinosis cutis. Given the prevalence among Africans of South African origin, there may be an underlying genetic component.
The causes of calcinosis cutis can be considered according to each type :
- Dystrophic :
– Acne
– Connective tissue disease
– Panniculitis – inflammation of the subcutaneous fat
– Skin infections
– Trauma to the skin
– Tumors
– Varicose veins
- Metastatic :
– Calciphylaxis
– Kidney failure
– Hyperparathyroidism
– Kidney failure
– Milk-alkali syndrome
– Paraneoplastic syndrome – where hypercalcemia and hyperphosphatemia arises
– Sarcoidosis
– Vitamin D excess
- Iatrogenic :
– Calcium and phosphate injections
– Repeated heel sticks (newborns)
– Electrode paste containing calcium (calcinosis cutis may only arise with prolonged use)
Idiopathic calcinosis cutis occurs for unknown reasons.
Diagnosis
Calcinosis cutis can be diagnosed by the physical appearance of the skin lesions in the backdrop of known hypercalcemia. Due to radio-opacity, the lesions may be visible to some extent on radiological imaging studies like an X-ray or CT scan. However, a definitive diagnosis can be reached with a biopsy of the lesion which is then examined under a microscope.
Treatment
Therapeutic measures should be directed at the underlying cause where possible. There is no definitive medical treatment for calcinosis cutis and surgical removal of the lesion should only be considered in severe cases.
Drugs such as corticosteroids, probenacid and colchicine may be utilized primarily for inflammatory conditions. Medication that can reduce deposits by disrupting calcium and phosphate metabolism includes :
- Antacids bind phosphates in the gut thereby inhibiting its absorption.
– Aluminum hydroxide
– Magnesium oxide - Calcium-channel blockers impair the entry of calcium into the cell thereby reducing intracellular crystal formation.
– Diltiazem hydrochloride - Calcimimetics acts on the parathyroid gland to reduce parathyroid hormone (PTH) which in turn decreases calcium levels.
– Cinacalcet - Diphosphonates slow down bone remodeling and calcium release from the bones.
– Etidronate disodium
Surgical removal of calcium deposits are reserved for lesions that are very painful, have ulcerated, have become repeatedly infected or hamper the functioning of certain parts of the body. However, there is a danger that excision of these deposits can stimulate further calcification. The recurrence rate after excision is high. Therefore excision should not be routinely conducted for calcinosis cutis. Electric shock wave lithotripsy (ESWL), the procedure which is used to “blast” kidney stones, may have some use in calcinosis cutis.
References :
www.dermnetnz.org/systemic/calcinosis.html
emedicine.medscape.com/article/1103137-overview
dermatology.cdlib.org/141/case_presentations/calcinosis/lobo.html