Venous Insufficiency of the Legs Causes
Venous insufficiency is a condition where the flow of blood from the leg back to the heart is impaired. The leg veins carry oxygen deficient blood away from the legs and certain anatomical features and physiological mechanisms in the leg enable the unidirectional flow of blood to the heart.
This includes the :
- Musculovenous pump (leg blood circulation pump) where the contraction and relaxation of the leg muscles during activity compress the veins thereby pushing the blood up the vessel. The pulsating of the leg arteries also helps to keep blood flowing in the veins.
- Valves in the leg veins prevent backward flow as the blood travels back to the heart. If blood attempts to flow in the wrong direction within the vein (away from the heart) the valve closes and prevents this.
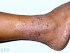
If the valves become incompetent, then blood may flow backwards (retrograde flow) and this is known as venous reflux. A blockage within a leg vein, usually by a blood clot, can also hamper the outflow of blood from the legs. Eventually blood will pool in the feet and lower legs and move very slowly or stay almost stationary. This sluggish circulation in the leg veins is known as venous stasis.
The vascular system is a continuous network. If the blood flow out of the legs are affected, then blood flowing into the legs will also be compromised and oxygen and nutrients cannot reach the tissue of the legs. Stasis of the blood also increases the chances of further and larger clot formation and eventually one of these clots can dislodge and block the arterial supply of a vital organ like the lung (pulmonary embolism).
Causes of Venous Insufficiency
The most common causes of venous insufficiency are varicose veins or a blood clot (thrombus more often, rarely embolus).
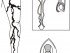
Varicose Veins
Varicose veins are enlarged tortuous veins due to pooling of the blood as a result of incompetent venous valves. The compromised vein cannot prevent the backflow of blood. As a result, blood pools in the lower parts of the leg, especially when standing. Varicose veins tend to arise in the following conditions :
- Pregnancy
- Inactivity – prolonged periods of sitting or standing
- Injury or infection of the leg especially if it affects the superficial blood vessels
Varicose veins do not arise suddenly. It develops over time and the symptoms appear gradually. It increases the risk of clot formation (thrombosis).
Thromobosis
A blood clot in the leg is more often due to a thrombus meaning that the clot forms at this site and can cause partial or even complete obstruction. With time, the blood cannot return to the heart efficiently and pools in the legs. Clots are more likely to occur in the deep veins of the leg, hence the term deep venous thrombosis (DVT). A thrombus may occur due to one or more of the following reasons :
- Cigarette smoking
- Inactivity – sitting or standing for prolonged periods and bedridden patients
- Obesity
- Use of oral contraceptives
- Shortly after childbirth
- Following surgical or investigative medical procedures that involves the leg or pelvis
- Heart failure
The risk associated with a thrombus in the leg is that it may dislodge, thereby becoming an embolus and ostruct a blood vessel elsewhere in the body, especially in a vital organ like the lung (pulmonary embolism).