Heart Failure (Left Side vs Right Side) Causes, Symptoms, Effects
What is Heart Failure?
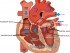
Heart failure refers to the syndrome that develops as a result of the heart’s inability to pump out enough blood to maintain an adequate blood circulation. In heart failure, the cardiac output is reduced and as the condition progresses, the body’s tissues become filled with fluid. This swelling or congestion of the tissue spaces (fluid overload) is the reason why heart failure is also known as congestive heart (cardiac) failure.
Most types of heart disease if left untreated can lead to heart failure. Many other conditions that directly or indirectly affect the heart can also result in heart failure. If these conditions can be adequately treated, heart failure can be halted. However, after a long period of time, the body’s compensatory mechanisms to maintain a normal cardiac output may cause irreversible damage to the heart.
What Happens in Heart Failure?
It is important to be familiar with the components and physiology of cardiac output in order to understand heart failure. Cardiac output is the amount of blood pushed out of the heart over a period of time. It can be measured by the volume of blood forced out of the heart during contraction (stroke volume) multiplied by the heart rate. Different conditions may affect the different components of cardiac output. The cardiac output is therefore reduced and the body utilizes a number of compensatory mechanisms in an attempt to maintain a normal cardiac output.
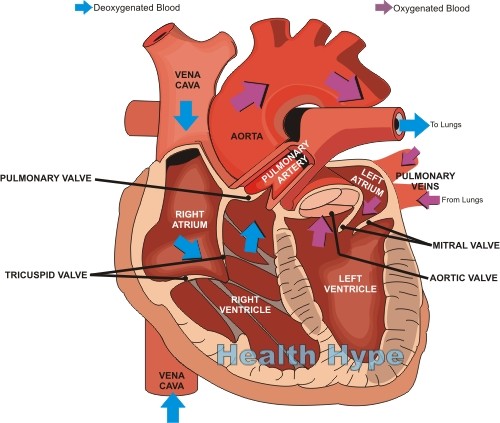
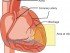
The heart has to fill with sufficient blood (end-diastolic volume) to create sufficient muscle stretching and pressure (preload) to ensure that enough blood is pushed out of the heart (stroke volume) to meet with the body’s needs. This is also determined by the strength of the heart muscle to force out blood (myocardial contractility) and the elasticity of the arteries, particularly the aorta, which need to stretch and recoil to keep blood flowing (Windkessel effect discussed under cardiac output).
In heart failure, cardiac output is reduced due to one or more of the following :
- Sufficient blood does not return to the heart and fill the ventricles (end-diastolic volume).
- Sufficient pressure and muscle stretching (preload) within the ventricles is not generated by the end-diastolic volume).
- Myocardial contractility is affected in that the heart muscle cannot generate enough force.
- The arteries lose their elasticity to keep blood propelled by recoil which reduces the blood returned to the heart.
Some of these factors overlap and eventually all will play a part in heart failure as these factors are dependent on each other.
Effects of Heart Failure
Initially, the body’s compensatory mechanisms attempt to stabilize the reduced cardiac output. A number of systems come into play in order to achieve these effects and maintain a normal cardiac output. None of the compensatory mechanisms can sustain the cardiac output over a prolong period of time and will eventually cause further damage to the heart and lead to heart failure.
The actions of these compensatory mechanisms causes the following :
- Decreased urine output so that the blood volume can be increased.
- Increase in blood pressure by causing vasoconstriction to return more blood to the heart.
- Increased heart rate to increase cardiac output.
- Enlargement of the heart muscles (hypertrophy) to pump with greater force.
- Enlargement or dilation of the ventricles so that more blood can fill into the heart.
Signs and Symptoms
The heart’s function is to keep blood circulated so that gases and nutrients can be transported to cells throughout the body. In heart failure this is not possible to the extent that it would be under normal circumstances. The consequence of this is :
- Exhaustion. Insufficient supply of oxygen and nutrients to the cells results in fatigue (low energy levels). In mild heart failure this may not be evident during rest but any exertion will quickly result in exhaustion.
- Shortness of breath (dyspnea). Water retention due to reduce urine output (explained above) causes fluid in the lungs (pulmonary edema) and around the lungs (pleural effusion) which affects gas exchange. This will also cause persistent coughing and abnormal breathing sounds like a wheeze. The shortness of breath is more pronounced when lying flat and sleeping (paroxysmal nocturnal dyspnea) and upon increased physical activity (exertional dyspnea).
- Edema. Pitting edema is commonly seen with swelling of the legs (peripheral edema), abdomen (ascites) or in severe cases, throughout the body (anasarca).
- Cyanosis. Bluish tinge of the skin as a result of decreased oxygen supply. This is more evident in the periphery (hands and feet) and initially the patient may only appear pale (pallor) due to reduced blood supply to the skin. The limbs are often cold to touch.
- Impaired mental faculties. Confusion, impaired cognitive abilities and a poor memory may be present as a result of the impaired blood flow to the brain and chemical changes related to the compensatory mechanisms.
- Arrhythmia. An irregular heartbeat may arise as a result of a prolonged increased in the heart rate which is one of the compensatory mechanisms.
Left vs Right Sided Heart Failure
Left-sided heart failure or left ventricular failure (LVF)is a reduction in the output from the left ventricle. The pressure in the left atrium increases as the oxygen-rich blood from the lungs are backed up since the left ventricle is not pushing out this blood fast enough or efficiently.
Right-sided heart failure or right ventricular failure (RVF) is a reduction in the blood output from the right ventricle. The pressure in the right atrium may be decreased, normal or increased depending on the return of blood from the rest of the body.
Left-sided heart failure is more common than right-sided heart failure. With time, both left-side or right-sided heart failure will lead to reduced cardiac output from both ventricles (biventricular heart failure).
Symptoms of LVF and RVF
| Signs/Symptoms | Left-Sided Heart Failure | Right-Sided Heart Failure |
|---|---|---|
| Pitting Edema (Legs, Hands) | Mild to moderate. | Moderate to severe |
| Fluid Retention | Pulmonary edema (fluid in lungs) and pleural effusion (fluid around lungs). | Abdomen (ascites). |
| Organ Enlargement | Heart. | Liver. Mild jaundice may be present. |
| Neck Veins | Mild to moderate raised jugular venous pressure (JVP). | Severe jugular venous pressure (JVP). Neck veins visibly distended. |
| Shortness of Breath | Prominent dyspnea. Paroxysmal nocturnal dyspnea (PND). | Dyspnea present but not as prominent. |
| Gastrointestinal | Present but not as prominent. | Loss of appetite. Bloating. Constipation. Symptoms are significantly more prominent than LVF |
It is difficult to isolate LVF from RVF based solely on the severity of jugular venous pressure (JVP), peripheral edema, shortness of breath or gastrointestinal symptoms. These signs and symptoms may vary among individuals depending on a host of other underlying factors.
References
- Heart failure. Medscape
Last updated on September 7, 2018.